Harried doctors and nurses, gowned in eerie layers, race to the call of codes. Hospital hallways overflow with the near-dead. Undertakers scramble to make space as body after body arrives, and refrigerated trucks are crammed with more, all waiting for some final bit of attention.
This is the gallery of suffering that seized headlines in the early months of the coronavirus pandemic, and then again during a winter surge in the U.S. Story after story peeled back on a health care system strained to the breaking point, from first responders in ERs and ICUs to last responders in funeral homes.
But what about the first first responders? Follow the thread of this frayed system, and you find ambulance EMTs — a legion of emergency medical technicians who are the low-paid but critical first line of defense in a crisis.
That’s the world Ava Kofman wanted to know about when she started to report “The Broken Front Line” for Pro Publica. Her 6,000-word narrative, published in April 2021, turns the spotlight to the foot soldiers of an ambulance industry that “has become a symbol of a catastrophe that has unfolded largely behind closed doors.”
Kofman spent three weeks embedded with two EMTs — Mike Diaz and Alexandra Sanchez — who work punishing 24-hour shifts shuttling patients to two hospitals that serve Antelope Valley (pop. 450,000), a suburban sprawl that is home to some of Los Angeles County’s “sickest and poorest residents.” Her assignment: “investigate the emotional toll of the cascade of structural failures on EMTs — an overlooked yet critical node of the healthcare system.”

Before joining ProPublica as a technology reporter in 2019, Kofman worked as a contributing writer for The Intercept, reporting on algorithms, artificial intelligence and surveillance technology. She mined the Edward Snowden archives to reveal the NSA’s pioneering use of voice recognition to spy on people, and disclosed how companies use AI to do risk assessments of employees by analyzing their voices. Her work has appeared in The New York Times Magazine, The Atlantic, Harper’s Magazine, The Guardian, and The New Republic.
Her data and research skills are evident in “The Broken Front Line.” She hunted down documents that confirmed long waits and backlogs at hospitals, studied medical literature on moral distress, and researched the history of LA County’s EMS system.
Traditional research and narrative observation
But the story is built on an impressive range of interviews and observation. She showed up for EMT shifts. Blocked by policy and privacy regulations, she couldn’t ride in the ambulances, so she trailed them in her car, often in the deep of night, and waited outside as EMTs triaged patients in their homes. On days her two main story subjects had off, Kofman reached out to other EMTs across Los Angeles to gain a fuller view of their world.
All that helped her get to the heart of her subjects, especially Diaz, a union official and who, at 31, is viewed as a father figure by his fellow EMTs. Kofman unspools the crushing burden of his care for the sick, and the toll it takes on his own sense of mission. Once he waits as long as 14 hours for a hospital to admit a patient. The description of Diaz’s interior mind is a tour de force of real-time reportage and narrative reconstruction that reveals, with withering clarity, a system overwhelmed by the pandemic.
Nieman Storyboard asked Kofman about her interview techniques, the challenges of pandemic reporting, and the way she chose, or “cast,” her main characters. Our email conversation has been edited for length and clarity, and is followed by an annotation of the story.
“The Broken Front Line” paints a vivid picture of the impact of the coronavirus pandemic on health care workers, told through two EMTs in a poor section of Los Angeles County. How did the story come about?
I started out with fairly open-ended reporting questions. As the U.S. reached the first anniversary of the start of the pandemic, how were these caregivers holding it all together? What systems, if any, were in place to support these workers if or when they were falling apart? And what might be the long-term psychological effects on them?
How did you find and gain access to the EMTs at the center of your story?
I called around a lot. I lost hope at one point, but my editors pushed me to keep trying a little bit longer. I was lucky to find EMTs who agreed that this kind of intimate story would be an important way to help the public understand the challenges faced by first responders. As COVID cases began to subside, Mike Diaz worried that people would conveniently forget that the hospital system had nearly collapsed. He saw a lot of value in making sure that we remembered the brutality of what had just happened.
Most of the story follows a familiar, real-time model: a day-in-the-life. Did you decide on that approach in advance and then do the reporting to gather the necessary material? Or did it emerge organically?
Real-time narration is inherently propulsive; it’s well-suited to the high-stakes drama of an emergency medical response. Before going into the field, I thought I might be able to tell the entire story through the lens of one 24-hour shift, or an especially long wait on “the wall,” which is what EMTs call the time spent waiting outside the hospital before their patients are admitted. Things didn’t work out that neatly, but having that initial structure in mind pushed me to look for moments of acute or prolonged crisis.
When the time came to stop reporting and start writing, I had no idea which scenes I’d choose, or how they’d all fit together. What I did know was that I wanted the episodes I selected to be representative of what Los Angeles EMTs had been experiencing throughout the second wave of the pandemic. Once I had selected those moments, I looked to familiar genres — like the “house call” and the “unfolding medical diagnosis” — to help me to block out the beats in each scene.
The depth of candor with which Mike Diaz described his thoughts is remarkable. What do you do as an interviewer to get people to open up with such depth?
Once I have done an initial “intake” conversation or two with someone, I tend to structure the rest of my interviews loosely or not at all; there will be few things I might need to ask about, but ideally, our time together unfolds according to our shared interests and curiosities. If someone is granting me the time to get to know them, we eventually get to all of the bullet points on my initial list; it’s far nicer if those topics emerge naturally or out of something they’ve just seen or we’ve experienced together.
To help generate descriptions, I ask subjects a lot of questions about how their world works and how they feel about it. I emphasize that I want to be able to explain things to people far away, and I often find this leads people to come up with interesting analogies and sensory details.
I also do a lot of background research; I’ll read or talk to secondary sources so that I can return to my subjects with increasingly specific questions or themes for us to talk through.
Journalist and teacher Walt Harrington once said that memory is a “sieve.” How could you be confident that you were reporting Diaz’s thoughts accurately?
Many of the thoughts included in the story were recounted or relayed to me in real-time, or something very close to it. The reported memories come from repeated interviews with Mike about events he experienced. For reconstructed events, I have confirmed details with additional sources whenever possible.
Your question seems to be getting at something larger, though, which is the fact that there’s always going to be some gap between what someone really thinks and what they tell someone they’re thinking. Also, what anyone really thinks at any given moment is mediated by whom one is with, the time of day, their mood, the setting, and so on. Our very presence as reporters might unintentionally shape a scene or someone’s recollection of an event. So far, it seems like the best workaround to these thorny epistemological problems is to have someone re-tell you something many different times, at many different moments; to respectfully press on different points of their story in each telling (i.e., Are you sure it was seven oxygen tanks? How do you know that?); to seek additional documentation whenever possible, and to triangulate details with additional eyewitness sources.
Are there writers or journalists that you draw on for inspiration?
I always return to Larissa MacFarquhar’s portraits of extreme idealists in “Strangers Drowning,” and they felt especially relevant to Mike’s story. To guide my observational reporting, I re-read Hannah Dreier and Eli Saslow’s immersive stories in The Washington Post. Rachel Cusk’s “Outline” trilogy, particularly the first two novels, helped me figure out how to place the right amount of present-day interjection and quotation within a reconstructed or recounted story. I also had the pleasure of reading John Berger’s “A Fortunate Man” for the first time this year. The book begins as a quiet portrait of a country doctor in rural England, then slowly builds into a philosophical treatise on the uncertain value of care-work in an unjust, uncaring society. As I was writing the story, I kept thinking about the last few pages of the book, where Berger seems to speak directly to the moral distress brought about by our country’s deadly mishandling of the pandemic. He writes this:
“One of the fundamental reasons why so many doctors become cynical and disillusioned is precisely because, when the abstract idealism has worn thin, they are uncertain about the value of the actual lives of the patients they are treating. This is not because they are callous or personally inhuman: it is because they live in and accept a society which is incapable of knowing what a human life is worth.”
For three weeks you were immersed in the misery that the pandemic inflicts on patients and the EMTs who care for them. How did you handle your own emotions?
I was definitely startled. I had never seen someone on a ventilator before, let alone a dozen people in a row tethered to these devices. But my overwhelming emotional reaction was stress: I was worried about writing a boring story that wouldn’t do justice to the experiences shared by my sources and to the suffering brought about by this unprecedented disaster.
The annotation: Storyboard’s questions are in red; Kofman’s responses in blue. To read the story without annotations, click the ‘Hide all annotations’ button, which you’ll find just below the social media buttons in the top right-hand menu, or at the top of your mobile device.
The Broken Front Line
As the winter’s surge of coronavirus cases overwhelmed Los Angeles hospitals, EMTs like Michael Diaz were forced to take previously unthinkable measures. What lasting impact will the pandemic have on America’s first responders?
by Kendrick Brinson and David Walter BanksApril 7, 2021
It was 4:32 p.m. and Mike Diaz was almost halfway through another punishing 24-hour shift when the call came over the ambulance radio. Nine miles away, a man had lost consciousness. “We’re en route from Palmdale Regional,” Diaz told the dispatcher, pushing away the thought of grabbing some food, as he flicked on the lights and sirens and sped off into the suburban maze of the Antelope Valley. He had worked as an emergency medical technician here in the northernmost part of Los Angeles County for over a decade, but he still experienced the same thrum of adrenaline on urgent calls. Lately, however, on January afternoons like this one, his excitement was overpowered by a sense of futility and dread. You start with one tight scene that has a lot going on. Help me unpack it a bit. First, were you with Diaz in the ambulance at the time? How much time did you spend riding with him and Sanchez?I did not ride inside the ambulance for safety, privacy and health reasons. I followed it around the desert in my own car as it responded to all of the calls described in the story. In the past, ride-alongs would be common for training purposes, for some media requests and, most crucially, for family members, but such opportunities were rendered too risky by the pandemic.You introduce your main character with a snippet of routine dialogue. Why did you select this quote?It seemed important to establish this beat of routine — a slice of the kinds of things EMTs normally do and say — before introducing the reader to everything that was unusual about this period of time. I also wanted to establish up top the leitmotif of the call-and-response dynamic with dispatch.How do you know he was pushing away thought of getting some food at that exact moment?It wouldn’t have occurred to me to ask about this kind of detail if I hadn’t been around to take in the rhythms of a typical shift. Their ambulance had initially been dispatched to “post” — that is, cover — at another station in Palmdale, and I knew from other instances that this might have been a natural moment to pick up food. I had been following him around all day and seen that he hadn’t eaten. But suddenly their rig got re-routed to an emergency call, so a break was out of the question. Later that day, and then again when I was fact-checking the story, I asked him about it.“Thrum” is a graceful noun choice, a hallmark of the story’s eloquent prose. When you report Mike Diaz’s thoughts, are they as accurate as a quote or did you give yourself freedom to paraphrase in your own language?While there are moments of free, indirect discourse throughout the story, the narration is not intended to continuously approximate any subject’s individual voice. The phrase “as accurate as a quote” strikes me as a little paradoxical — or rather, counter-intuitive — as I tend to think that quotes are not necessarily the most accurate way for the writer to convey her subject’s emotional reality. A quote rarely synthesizes hours of deep conversations, not to mention the mass of other information beyond those interviews, such as the reporter’s own observations and reflections, testimony from other sources, documents, photographs, and so on. Ideally, a story’s authoritative narration is produced from synthesizing all of these inputs.Do you follow any guidelines when you decide to paraphrase rather than quote?I don’t have strict guidelines, but I tend to prefer to use quotes to give a sense of how someone speaks or thinks. I also enjoy quotation when trying to convey the particular intensity of a recounted experience or needing to express someone else’s argument. When I do choose to convey someone else’s subjective reality through paraphrase, however, it’s important that my writing remains factually accurate to the subject’s thoughts or feelings as they were recounted to me. In my fact-checking conversation with a source, I’ll usually say something along the lines of, “You told me you felt or thought XYZ and I describe XYZ by saying ABC...” If any of this paraphrasing strikes my sources as inaccurate or off, I’ll refine it until it rings true.
A few minutes after the dispatcher’s call, Diaz backed the ambulance into the driveway of a single-story house with a white picket fence. You pick up the scene almost immediately after the call comes. Why did you leave out whatever happened between that and their arrival? How do you decide what to keep or leave out from all the things you learn? The drive to the patient’s home took just under ten minutes. I did not consider using that drive since I wanted the pacing to be tight; the goal of this scene was always to quickly reach the patient and, not long after, the gridlock at the hospital. Overall, when making choices about cutting in and out of scenes, I try to imagine each paragraph as a photograph or a frame from a film. Each scene needed to reveal a different part of the larger story about the challenges of this work during the winter surge. I don’t have a very formal outline process, but I tried to think about illuminating different emotional states (a sense of moral purpose, trauma, monotony, stress, and so on) in each section of the story. He and his partner, Alexandra Sanchez, followed a paramedic from the fire department into a dim living room, where an old man was stretched out on a cot, grimacing in pain. How did you select Mike Diaz as your main character?In his role as both a veteran EMT and a union leader, Diaz had an unusually panoramic view of the emergency medical system. He was a knowledgeable guide to the system as well as a candid observer of the field’s many issues, including those that had existed long before the pandemic. His stakes were especially high: He was fighting not just management but management’s response to the pandemic. I was lucky that he allowed me to shadow him and then to meet his partner, Alexandra. As I learned about their experiences, I realized that this was not just a story about EMTs confronting the mass suffering of patients in the pandemic. It was also a story about how they were having to confront their inability to help all of the patients they encountered. As Diaz crouched to check the man’s vitals, a middle-aged woman said that she had first noticed her father, who was 88, becoming less coherent around a week ago. The man was more confused than usual, and contractures had stiffened his thin legs into tent poles. The description of the elderly man’s thin legs “stiffened into tent poles” is so painfully vivid. Is that the kind of detail that goes into your notebook at the time, or does it surface later, during writing and revision?I had glimpsed the patient’s legs at the hospital. Later when I sat down to write, I searched for a phrase that would help visualize their brittle, modular arrangement for someone who didn’t know what the word “contractures” meant or had never seen them. Their primary care doctor wasn’t picking up the phone. Still, the family held off on dialing 911 because they feared that sending him to the hospital would expose him to the coronavirus. Only now that his condition had worsened had they decided to make the call.
As the daughter spoke, Diaz uttered short affirmative phrases.I’m curious why you didn’t quote Diaz or any of the specific phrases.I did not enter the patient’s home, so all I had access to here was the contours of a recalled conversation, rather than actual dialogue. From spending time with Diaz, I knew he was an unusually attentive listener. He has these little nods and minor catchphrases — “Correct.” “Absolutely.” “Factual.” “Uh-huh.” — that gently stream out while someone else is speaking. I asked him later if he was listening in this fashion, as he usually does, and he said he was. At 31, he is brawny and compact, with a smooth face, alert eyes and spiky black hair that lends an extra inch to his height. How much time did you spend with Diaz before you were able to write this description?Since physical description is based on the reporter’s observations, and not as much on any special access, it probably could have been written after 30 minutes of reporting. I tend to write physical descriptions at the very end because I find them challenging and I’m trying to find the least obtrusive space to slot them into the draft. He was used to the brutal rhythms of emergency medicine in the Antelope Valley. The bustling community of 450,000, an hour’s drive north of Los Angeles, has only two hospitals and some of the county’s poorest and sickest residents. Diaz was overworked and proud of it, driven by the intoxicating rush of saving lives. Were these Diaz’s words?They’re a faithful summary, yes. Drawn from our various conversations, this broad sketch synthesizes some of the very first things Diaz told me: the busy-ness; the two hospitals; his idealism, and just how far his hopes had been tested and degraded. Even when the 911 system was under strain in the past, he could take for granted that there would be enough resources — supplies, space and staff — to tend to patients. What he lost in sleep and free time he’d always earned back in the satisfaction of helping people. In a job that paid low wages and demanded extreme sacrifice, he’d come to rely on that feeling.
Now he could no longer count on it. The recent explosion in coronavirus cases — an over 900% increase in LA County from November to January — had left the health care system on the verge of collapse. Here you smoothly set up the contrast of the days before the pandemic struck and what followed when it descended on Los Angeles County, as well as describing Diaz’s work ethic. How much time did you spend drafting and revising the passage?I normally spend about half of the time I’m allotted for my first draft — sometimes a little more than that — figuring out the story’s opening beats. There were so many stories about the effects of the pandemic. I wanted to be clear right at the top that this was not another story about patients, or hospitals, or the general disintegration of the healthcare system. In this new climate of scarcity, the more people there were who needed help, the less EMTs could do to help them. Peering down at the pale old man before him, Diaz was gripped by doubts: Could he still call himself a caretaker when he couldn’t properly care for his patients? Here you seem to establish the central focus of the narrative, dramatized by the doubts Diaz felt. Was that the goal?Definitely. This was something that Diaz spoke to me about in our first conversation. Many of the other EMTs I spoke to also discussed the jarring transformation of their role, with its diminished scope and expectations, making them feel as though they’d lost their sense of purpose and identity.
Ten minutes later, as he swung left into Antelope Valley Hospital, Diaz was dismayed to note the first signs of gridlock: Five ambulances were already parked in the bay. Diaz and Sanchez wheeled their patient toward the back entrance of the emergency department, where they joined a phalanx of other gurneys. Tell me about your choice of “phalanx,” which usually has military connotations, to describe the ER that night?I had in mind the secondary definition, which is a group of similar things forming a compact body. Emergency medicine first originated as a way of treating wounded soldiers on the battlefield. During the recent surge, it seemed closer than ever to these wartime roots with EMTs, as Diaz put it, occupying “the front lines of the front line.” A mother and her crying infant. A man whose legs had swollen up like the limbs of a balloon animal. While writing. A woman whose wrists were in restraints. She’d spat at the EMTs who’d brought her in and, because they couldn’t find a mask, they’d placed a white napkin over her face. This litany of needy patients demonstrates what writing coach Roy Peter Clark, in his book “Writing Tools,” calls “the power of three….We use one for power. Use two for comparison, contrast. Use three for completeness, wholeness, roundness. Use four or more to list, inventory, compile, and expand.” Did you have that theory in mind when you made the list of the three patients?I was not aware of these great rules, but I’ve always been fond of listing things in groups of three for the reasons you describe. “It looks like it’s one of those days,” Diaz said. Who was he speaking to?This was probably something he was thinking to himself but had vocalized for my sake, since he was serving as my guide to the chaos. He made this remark as he pulled up with the gurney and saw the crowd.
In the alcove beyond the check-in desk, Sanchez and Diaz installed their gurney along a vacant stretch of beige hallway. Before the pandemic, an 88-year-old man in an altered state of consciousness would be attended to fairly quickly to rule out an infection, prior brain injury or stroke. Who told you this?The EMTs and, later, medical professionals who I consulted while fact-checking. Today, every bed in the ER was occupied, and Diaz and Sanchez had been relegated to the limbo known to EMTs as “the wall.” The term refers to the uneasy period of waiting with a patient until a bed becomes available. Even in quieter times, it was common in the Antelope Valley to “hold the wall” a few times a week. But now crews were waiting to offload patients two or three times a day, and the waits kept getting longer. A few weeks earlier, Diaz had been on the wall at Palmdale Regional Medical Center for 14 hours straight. Around Christmas, Sanchez had dropped off a patient only to see the person still waiting for a bed on her next shift, 30 hours later. Someone had etched tick marks onto one of the hospital’s corridors, like an imprisoned soldier counting his days in captivity. When did you learn about the term “the wall” and the phrase “to hold the wall,” which are such powerful, dispiriting details?The term is ubiquitous in the field of emergency medicine. I heard about “holding the wall” during my very first conversation with a different EMT. “The wall,” it seemed to me, was not only an activity but a great synecdoche for all of the failures and impracticalities of how emergency medical care is organized in this country. It’s always been slightly awkward to have EMTs wait around to formally hand off patients to nurses, since it renders their ambulances unable to respond to other emergency calls. In the pandemic, however, this arrangement became untenable, since crews were serving as de facto hospital staff for marathon stretches at a time. Before I went out into the field, I thought perhaps that the entire story would take place “on the wall,” given all of its symbolic resonances. But that initial idea changed in the course of my reporting, as initial ideas so often do!How did you know about the “tick marks?”I saw the marks, which seemed to underscore the atmosphere of helplessness. When something seems striking, I’ll try to snap a photo on my phone. I then go through these visual notes along with my written notebooks and iPhone notes when collating my materials for the drafting stage. The imprisoned soldier comparison came to mind when I first noticed them. Given how powerless everyone felt — and the sort of improvisational, wartime roots of the profession I mentioned above — it seemed apt.
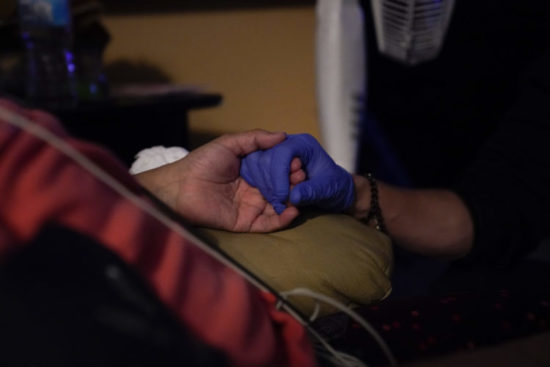
Diaz noticed his patient was struggling with a pair of blue gloves. “I’ll help you put those on if you want, sir,” he said. “Just let me take your temperature.” His gestures were attentive, precise.
The glass doors of the ER slid open and another EMT poked her head through to scan the crowd. “It’s a party in here,” she said, before returning outside to tend to a heavyset man who was shaking uncontrollably.
“Is your pain still a 10 out of 10?” Sanchez, who is 26, asked their patient. She has a radiant complexion and a serene bedside manner.
“I can’t hear you,” he said. Down the hall, a heart monitor pinged. The infant continued to wail. The sounds act as a kind of chorus to the specifics of an intimate scene.It seemed important to recreate the sensory experience of being on the wall for someone who hadn’t seen it before. The idea of noise was already being introduced by the scene — with the patient stating that he was having trouble hearing — so it seemed like a natural spot to note these details.
“Your pain,” she said, raising her voice above the din. When she leaned over him, her ink-black bangs hung above her mask. Why include this bit of description?It seemed like an unobtrusive place where I could provide a little more physical description of Sanchez. Plus, the image of a masked face is not exactly the most cheering vision for a patient already hard of hearing and suffering from confusion. “Still a 10 out of 10? Is your pain still really bad?”
She couldn’t tell if he was nodding in agreement or simply adjusting his head. Either way, there was nothing to do now but wait.
In just 482 words, this dramatic scene, a resumption of the lead, conveys a health care system under collapse from an unrelenting virus. How much reporting did you have to distill to write it?It took a while to figure out which scenes to choose, but once I selected this one, there wasn’t an enormous amount of material to distill. It was more a matter of fine-tuning the elements that would economically convey the story’s themes. You use unforgettable description and what James B. Stewart in “Follow the Story: How to Write Successful Nonfiction,” calls “narrative quotations — statements made at the time of the events being described,” as opposed to “contemporary” ones “made later, usually in a response to a reporter’s questions.” Do you use a notebook, audio recorder or both?Both, whenever possible. Also, iPhone notes to discreetly transcribe overheard exchanges.
With its flashing lights and whooping siren, the ambulance has become a symbol of a catastrophe that has unfolded largely behind closed doors. At the start of the pandemic, Diaz hoped the elevated profile of EMTs — their “essential” role — might lead to improvements in the way that emergency medical services are run. But so far, nothing had changed. If anything, the situation had gotten worse. The voice changes in this section, shifting from dramatic to summary narrative that sets the personal stories of Diaz and Sanchez against the larger context of an ambulance industry in crisis. It tells, rather than shows. Do you consider it the story’s nut section?Definitely. The first “topic” or “transitional” sentence into this section indicates that the focus of this story is not so much the hospitals or the patients, but the role of ambulances and their crews. The ambulance sits at the crossroads between the hospital and the public. I wanted to remind people that its prominence in daily life is symptomatic of the healthcare system’s collapse. In order to show how the system fell apart, I had to first suggest how the system was glued together. Also, I felt that most people wouldn’t know much about how the ambulance system worked beyond the fact that it gets you to a hospital. I’d initially tucked different parts of this information throughout the story, but fairly late into the revision process, I decided that my approach was ineffective at best and confusing at worst: it made more sense to group the details in one place, so that we could understand how Diaz and Sanchez’s lived experiences fit within the larger health care system in which they worked. It would have been strange or misleading to mention that Diaz and Sanchez worked for a private ambulance company without explaining that emergency medical systems are privatized in many counties across the US; and it seemed crucial to zoom out and note that EMTs were stretched thin outside of LA, too. By zooming out, one could take in the structural forces that EMTs are up against all at once, which, ideally, establishes the dramatic stakes for the rest of the story to elaborate on.
In Los Angeles County, as in many parts of the U.S., for-profit companies operate the ambulance system. The contract for the north part of LA is held by American Medical Response, the largest ambulance company in the nation. Along with paramedics from the fire department, EMTs employed by American Medical Response handle all of the emergency medical calls in this “exclusive operating area,” a roughly 1,500-square-mile dominion that includes the cities of Palmdale and Lancaster, a smattering of quarries and aerospace factories, and swaths of the Mojave desert.
Spending as little as possible is crucial for all parties involved. The government, which pays for the majority of ambulance trips in many parts of the country, wants to save money. And AMR, of course, makes more if it keeps costs down. Diaz is particularly attuned to this dynamic: He represents around 350 AMR employees as president of an EMT union’s local. Although this section departs from the scenes of the opening, Diaz still makes an appearance.Diaz understood himself as caught at the center of this business model. He was well aware of how financial realities contributed to working conditions that some of his members found constraining. This seemed like an expedient way to tie these abstract structures to the lived experience of someone we have already met in the story.
Los Angeles County mandates that ambulances reach patients within 8 minutes and 59 seconds. Why the precise time measure?Ambulances need to get to the scene as soon as possible in case of emergency, and in urban areas, the majority of their responses must meet this deadline to avoid fines. In rural tracts, the deadline is 20 minutes and 59 seconds. Crews regularly update dispatch on their location and timing; the whereabouts of crews can also be monitored through GPS. To meet this deadline while maintaining profit margins, private companies deploy a thin fleet of ambulances, pay low wages (private-sector EMTs in California make 39% less than their public-sector counterparts) and strategically rearrange the vehicles in their command. AMR’s software suggests that vehicles “post” near busier areas so they’re more likely to encounter transport opportunities. On hectic days, dispatchers maneuver crews around like chess pieces. Where did that comparison come from? I spoke to four dispatchers and two supervisors. The idea of arranging crews on “a chess board” came up twice in those conversations.
“We’re not unlike other parts of emergency health care — we’re very lean,” said Tom Wagner, president of AMR’s western operations. “When dollars are tight,” he said, citing low Medicare reimbursement rates, “decisions have to be made about where we station ambulances, how we station ambulances, and do we move them around more often?”
In all, how much time did you spend on the story?I was assigned to look at how the winter surge was playing out for caretakers in Los Angeles at the start of January, though at that point it wasn’t necessarily clear that I’d be focusing on EMTs. I worked on the assignment until it was published on April 7. What role did your editors play?My brilliant editor Nick Varchaver made sure that this intimate profile would also come across as a portrait of an entire profession under duress. We had many big-picture discussions about the story’s mood and moral themes, as well as how to balance contextual beats with the narrative elements. He encouraged me to widen the story’s frame at several key moments and pressed for nuts-and-bolts explanations of important details that I had rushed over or neglected to mention in earlier drafts. The wave of coronavirus cases that swept across the country late last year put even the most battle-hardened EMTs under unprecedented psychological strain. “All of the structural shortfalls of our industry were really borne by EMTs and paramedics who were at the patient’s side, caring for them without the resources that they needed,” said Aarron Reinert, who until recently served as the president of the American Ambulance Association, an industry trade group. Some companies, he said, lost money early in the pandemic when many people were reluctant to go to the hospital; other companies, faced with a surge in cases, ran out of masks, gloves, medications, syringes, vehicle parts. In late November, the association sent a letter to the U.S. Department of Health and Human Services, pleading for more government aid. “The 911 emergency medical system throughout the United States,” it stated, “is at a breaking point.” Did you talk to the agency about this?HHS doled out aid early on in the pandemic through the Provider Relief Fund. An HHS spokesperson provided me with general background information that did not directly speak to the complaints raised in the letter.
A few days later, in Los Angeles, it broke. You follow the quote about the system breaking down, followed by this terse, nine-word sentence. Why?This sentence was meant to work as a funnel that would shuttle us from this national view to the story’s regional focus: the breakdown in LA.
The more critically sick patients dialed 911, the more intensive care unit beds filled up; soon, those ICU patients were overflowing into the emergency room and EMTs had to wait for hours to offload newer patients until others were discharged or died. With so many crews stuck on the wall and several dozen more in quarantine or sickened by the virus, there were fewer and fewer ambulances on the road to handle all the 911 calls, which led to dangerous delays in emergency response times. With each passing day, the situation deteriorated. Hospitals assembled disaster tents and installed mobile morgues. Eventually, dispatchers were making informal triage decisions about where to send the last available ambulance. Here you take just 115 words to describe a harrowing state of affairs. How do you achieve such economy?There’d already been a steady stream of reporting about every element of this disaster as it unfolded in Los Angeles. But most of it had not been from the point of view of the ambulance system. I was struck by the fact that the EMS system was both a catalyst and a casualty of this breakdown, and I wanted to re-narrate the catastrophe through that lens. To write this paragraph, I drew a circle on a piece of paper and mapped out the different parts of this negative feedback loop. It’s against this backdrop of progressive deterioration that the action in the story takes place.
To combat this vicious cycle, EMTs like Diaz and Sanchez were forced to do things they’d never done before. They stayed awake for 48 hours at a stretch, piled on extra shifts to cover for sick colleagues, and brokered final goodbyes between patients and their loved ones. To free up ambulances to run other calls, they attended to groups of patients. Some patients on the wall had been passed between so many crews that their latest handlers scarcely knew what they’d come in for. All that mattered was ensuring that the person kept breathing. In the midst of this context situation, Diaz and Sanchez both reappear in a detail-rich and gracefully written passage. Embedded in the context section, it seems to stand outside the narrative sections of the work they perform. Why did you bring them back on stage?They re-appear here to represent what many EMTs were resorting to throughout the pandemic. The subject of this paragraph is EMTs more broadly — EMTs like them — to make it clear that while this was a story about two EMTs, their experiences were in many respects representative of what the profession was going through in Southern California. The reporting was informed by interviews with two dozen EMTs.
High-flow oxygen, sent through the nose, is effectively the only stabilizing treatment that EMTs can administer to people infected with the coronavirus. COVID-19 patients can require 10 times the amount of oxygen of non-COVID-19 patients, How did you learn this?Expert interviews, including with the medical directors of the county and the city’s fire departments, respectively. and as demand soared, ambulances and hospitals ran through their supply. At the start of January, the county’s emergency medical services agency instructed EMTs and paramedics to withhold oxygen from those whose blood oxygen saturation was above 90%. (Typical blood oxygen levels range between 96% and 100%; levels below 90% can be cause for concern.) Why did you isolate this information between parentheses?The fact serves as an additional beat of context for the previous sentence.
Some of Diaz’s patients appeared to be suffocating, but so long as their blood oxygen saturation was above the threshold established by the county’s much-needed rationing protocols, he had to deny them. People gasped and heaved and moaned. It made him feel like he was watching someone drown. Once again, you present Diaz’s interior thoughts. Why did you paraphrase instead of quoting him directly?This was the most direct way to present his experiences and synthesize his account. These were experiences we had talked about in our first phone call and returned to over the course of many conversations. Sometimes quotes can be distracting or give too much attention to a specific interview that took place at a specific time. But also, in this case, I tried to limit myself to live dialogue (i.e., narrative quotation) as much as possible to amplify the story’s immediacy and urgency.
The rationing was even more upsetting for the patients themselves. They were shocked — rightfully so, Diaz thought — by what was happening. This is America, they told him. This is California. These expressions of disbelief, Diaz observed, were often followed by anger. One of his patients, desperate to see a nurse, called 911 from inside the hospital. Others called him names. He understood their frustration. He was frustrated, too. How could he convince someone whose lungs were filling with fluid that he actually wanted to help them when he was mostly just standing there? How close in time were the scenes you witnessed and the conversations you had with Diaz to learn what he was thinking?Very close in time. We also went over conversations and reflections in the fact-checking process. Given his frenetic schedule, how were you able to gather so much material in addition to the on-scene reporting? Did you continue to interview him after the three weeks you spent with the EMTs had ended? If so, were these in-person, or other means (phone calls, emails, texts)?By the time I arrived, the curve of cases had begun to slope downward. There was some downtime at the station where we could chat for stretches in between calls. We also met on his day off, talked on the phone, and emailed and texted about smaller details.
As the sun set on Antelope Valley Hospital, more EMT crews arrived, joining Sanchez and Diaz on the wall. They exchanged mordant greetings. Here you return to the story’s day-in-the-life structure, using the sunset to convey the passage of time. Why did you choose nature over clock time?I wasn’t referring to a specific or discrete timestamp here, so I needed a marker that would convey a broader period of time. These snatches of dialogue happened over the course of the sun going down.
“Fancy seeing you here!”
“Where have you been all day?”
“Welcome to zero space.”
The line of gurneys had spilled beyond the doors of the ER, into the cooling night air. EMTs wrapped their patients in coarse white blankets. Nurses wheeled equipment out onto the pavement to take vitals. Diaz and his colleagues milled about. I admire the way you consistently use series of subject-verb-object sentences to convey a mixture of actions that reveal scenes with such economy.Thank you. As a reader, I’ve found that a well-chosen verb can do a lot more descriptive work than a whole string of adjectives.
As the union leader, Diaz was highly sought after by his fellow EMTs. He made his rounds with the easygoing self-assurance of a man who delights in fixing peoples’ problems. One EMT flagged him down to say that he was worried about disciplinary action following a dispute about attendance. Diaz reassured him that the matter would be dropped. Another EMT said she was working overtime to pay her bills after calling out with COVID-19 at the start of January. Diaz told her he’d file a grievance and find out why she hadn’t received sick pay. (AMR’s policy is to compensate coronavirus-positive workers until they test negative.) Was this happening in the scene at the ER? If not, were you concerned about interrupting what the novelist John Gardner called the “vivid, continuous dream” of storytelling that captivates readers?Ack! This was all happening in the same scene in the ER. I should have made that clearer. I had originally included all of the back-and-forth dialogue that took place in each of these exchanges, but the scene had started to drag. Since the point I was trying to get across here was that Diaz was serving as a caretaker to both his colleagues and patients, I decided that it was more efficient to tell directly here rather than to show.Just curious: What’s the ProPublica style rule for using parentheses?I am not sure. I hope there isn’t a strict one!
In the sea of crisp navy uniforms, Great image! Did you come up with it on the spot?No, I put this in at some point during the revision process, when I was thinking about how to add more “color” to my description of the wall. Diaz spotted his buddy Gage Oldenburg, a 24-year-old EMT with a bristly blond mustache. Why out of all the aspects of his appearance did you choose his facial hair? I tend to go with whatever feature I find most memorable or striking, assuming that whatever has stuck with me will also be vivid to someone else. Plus, if everyone is wearing masks most of the time, and in this case, the same uniform, hair is one of the few prominent and distinguishing features. In my fact-checking process, following the rule of “no surprises,” I try to alert subjects to whatever physical descriptions of them are in the story. They chatted about the frenetic pace of work. For most of January, there’d been more than 200 coronavirus deaths a day in Los Angeles, the equivalent of one death every seven minutes. Why did you follow the number of daily deaths with the rate-per-minute?It was such a vivid analogy that so many public health officials were using at the time. It had helped me to comprehend the extent of the virus’s destruction, so I figured it might help others, too. No one — not their supervisors, not the fire department chief, not the doctors in the hospital — had ever seen anything like it. EMTs and paramedics already suffer disproportionately from post-traumatic stress disorder and suicidal ideation. What the effects of the pandemic will be on these first responders in the months to come remains to be seen. “This took an emotional toll that we will probably be seeing for years,” said Cathy Chidester, the director of LA County’s EMS Agency, which oversees the ambulance system.
Many EMTs are on duty in 24-hour shifts, but before the pandemic, there were plenty of opportunities at the station to nap, decompress or console one another about harrowing calls. On days off, Diaz, Oldenburg and other AMR friends camped on the beach together, watched Lakers games and grabbed mimosas in the early morning after work. Once the rise in hospitalizations put an end to all downtime, though, these bottlenecks at the hospital had become one of the few occasions where crews could process the unfolding disaster. “It used to be that people enjoyed their jobs, even though there were parts they didn’t enjoy,” Oldenburg said. “Now a lot of people just show up because they feel like they have no other option.” Why did you limit interior monologues to Mike Diaz?I suppose because looking over someone else’s shoulder might have seemed confusing or raised more questions than it helped to answer.
Diaz did his best each shift to keep morale up. He liked to remind his colleagues that they were “on the front lines of the front line.” Yet even he’d found himself becoming inured to scenarios that would have been previously unthinkable. He no longer noticed when every patient in the emergency room was intubated. He was indifferent to the high-pitched ring of the alarms that signaled the end of the hospital’s oxygen supply. Of course, some detachment was natural, even necessary, in a profession that routinely deals with the worst day in someone else’s life. But it wasn’t just that he was desensitized; sometimes he had trouble feeling anything at all. This is devastating. What was your reaction when he told you this?One night we had seen something that I had found disturbing and I asked Mike about whether it was disturbing for him well. He said it wasn’t, and that he’d become desensitized to those sorts of things. So then we talked more about that — and about whether 2019 Mike would have been shocked by what 2020 Mike was seeing.
Shortly after 7 p.m., while Sanchez watched their patient inside, Diaz bolted down a beef bowl from a local fast-food chain using the hood of an ambulance as a table. It was his first meal of the shift. He and Sanchez had been running calls — a cardiac arrest, a dirt bike accident, a COVID-19-positive woman with a blood clot in her leg — since 6 a.m. At one point, they’d had to drive through an hour of traffic to cover a station down in Santa Clarita because too many units there were tied up or out sick. How do they maintain their stamina?A lot of energy drinks. There are also all kinds of tricks for staying awake on no sleep: driving with the AC on when it’s already cold outside or blasting the heat if it’s a scorcher; slapping one’s face; putting on loud music; alternating between different sources of caffeine (coffee, espresso, RockStars, RedBull); chewing nicotine gum.
“This is a good day,” Diaz said to Chris Canning, a jovial EMT who wore his hair pulled back into a small bun. Again, why this bit of physical description?Hm. Now that you mention it, it would have worked just as well to cut this physical description. It’s a vestige of an earlier version of the story, when this dialogue had been part of a longer exchange. Diaz was so accustomed to the chaos of the surge that an unscheduled break during a shift of nonstop calls now seemed like a luxury.
n his happiest moments, Diaz would tell himself, “I’ll do 30 years and call it.” He loved his job. He was good at it. His life as an EMT was more exciting, more significant and more satisfying than anything he had previously done. Why not keep at it for decades?
Some people enter emergency medicine because they’ve witnessed a paramedic saving the life of an uncle or mother. Or because a relative died before help arrived and the future medic wishes to prevent the same thing from happening to someone else. Others, teenagers just out of high school, drive ambulances before moving on to higher-paying jobs in medicine. An EMT certification is also a prerequisite for joining LA’s highly selective fire department.
Diaz did not want to be a firefighter and he had not lost a family member through a catastrophic event. Rather, he had fallen in love. He was interested in a girl who was interested in another guy. The other guy was an EMT. Diaz didn’t see why he couldn’t do the same thing his rival did, “but better.” When I worked in the features department of the St. Petersburg Times with Tom French, the Pulitzer Prize-winning narrative writer, he used to talk about “auditioning” potential subjects to decide which would be the most compelling characters? Do you do anything like that?Yes, I engaged in a “casting process,” which involved speaking and meeting with several EMTs before settling on Mike and heading out to the Antelope Valley. But even after my reporting narrowed its focus, those other conversations informed my understanding of the story, the right questions to ask, and how to accurately frame the story. All that research gives me a sense of what’s normal, what’s abnormal, which views are idiosyncratic to my subject or shared widely by colleagues in the field. At the time, Diaz was studying film at California State University, Northridge and working as a projectionist at a movie theater. Between classes and work, he attended a 12-week EMS course and flunked out. “My mind wasn’t in the right place,” he realized. “And then I was like, wait, why did I fail that?” At first his pride compelled him to try again, but he was soon transfixed by what he was learning about the human body’s extraordinary ability to compensate for its injuries and illnesses. Though he eventually lost the girl, he gained a vocation, and, in 2009, at the age of 20, he joined American Medical Response. Why did you choose this point to present Diaz’s backstory?The start of the story talks a bit about Diaz’s commitment and motivations — about the fact that he’s driven by the “intoxicating rush” of helping folks — but it was important to explain his initiation into this world and his motivations for joining it. As a reader, I always find that these initiation sections — the parts of the story where you learn about why someone came to care or feel a certain way about what they do or who they are — deepen my sense of investment in the subject or character and in their cause. Ideally, those sections of backstory serve to initiate the reader by taking them along the journey to the present day.
The first year of work was so humbling and surprising that he started to tell people that every 18-year-old should spend a year in the front seat of an ambulance. He imagined a compulsory EMT service, like a military draft. It wasn’t just that the world needed more EMTs, in his view. It was that he could think of no other job that put one’s own life into such sobering perspective.
To be an EMT is to understand a truism that might otherwise seem abstract: Someone, somewhere is always suffering.I was struck by the wisdom and compassion of this observation. Did Diaz tell you this or was it your conclusion?The more I traveled to calls, the more I started to learn about how the grid of a city might look and feel to an EMT. From their point of view, there’s always another calamity just around the corner. Every building, every tract house and shopping center and nursing home represents a potential source of injury and sorrow. This intimate relationship to disaster was something that struck me one day while driving to yet another call, and I said it into my recorder so I wouldn’t forget it. Then I asked EMTs if it checked out with their experience. Once he tuned in to the frequency of disaster, Diaz found that trivial frustrations no longer bothered him. Life’s smaller pleasures became more fulfilling. Other people might have been disheartened by such unrelenting proximity to pain, but the knowledge that things could be worse filled Diaz, a relentless optimist, with a profound sense of calm.
As the years went by, however, Diaz noticed that he was working with fewer and fewer of the people he had started with. His colleagues around the station were always asking each other about their next move. Fire? Nursing? Law enforcement? He dreaded these questions, which implied that their current career was lacking. The low pay, long hours and high turnover rate only reinforced this impression. Even his friends who adored the EMT lifestyle, with its sense of purpose and foxhole camaraderie, usually ended up leaving after two or three years. Did it really have to be this way? Diaz wondered. Why couldn’t working as an EMT be a sustainable career in itself? Why was it important to paraphrase or summarize his inner thoughts here, rather than quoting him?These questions are always rolling through his mind. They’re his engine: what he continually asks himself and his colleagues as he pushes for change.
In the summer of 2017, eight years into his tenure, Diaz ran for president of Local 77 of the International Association of EMTs and Paramedics. Wages were a consistent matter of concern. As one of the most senior employees in the area, Diaz’s hourly wage is $17.89, while Sanchez, after four years at AMR, earns $15.88 an hour. No one got into EMS for the money, as the saying around the station went. Then again, the industry appeared lucrative for those higher up the food chain than Diaz: AMR is a subsidiary of the $4 billion Global Medical Response, which in turn is controlled by KKR, a $252 billion private equity behemoth. (AMR’s Wagner emphasized that hourly rates are established through the collective bargaining agreement. “We are constantly looking at ways to be able to adjust compensation,” he said, “because we’re only successful if we have people that want do the job and be aboard our team.”)
Diaz threw himself into the union cause. If burnout was built into the job, he wanted at the very least “to go down swinging.” His response to the pandemic was to push himself even harder. He filled his days off with overtime shifts, filing grievances on behalf of members and recording livestreams on Facebook to address safety concerns. His phone rang throughout the night with colleagues seeking advice. He always picked up.
Everything was urgent. He was needed constantly. He could not stop to rest, to sleep, to eat. His girlfriend called him Zombie Michael. But he insisted he was fine. He was fine. Really.
Until he wasn’t. One night in the middle of December, Diaz was walking down the hallway at Palmdale Regional Medical Center, when he noticed that oxygen tubes had been recently taped along the ceiling. The hospital had exhausted its portable tanks, and the new lines were rushing oxygen from exam rooms to the row of rasping patients on the wall.
It was strange, but as he stared at the taped tubes, the image of scarcity elated him. At that moment, he felt that the only hope for transformative change to the health care system would be if the absolute worst finally came to pass. He imagined what would happen if 30 more people with COVID-19 flooded through the door. If they quit rationing and just ran through the entire oxygen supply. If hundreds of people died that night.
Diaz began to clap, as though he were cheering on a basketball team. “Let’s go,” he said, raising his voice. “Let’s do it! Let’s break the system!” He was strolling down the hall now. “Let’s bring more patients in,” he said, clapping his hands more forcefully. “Let’s put everyone on two more liters. Let’s just break it.”
His euphoria lasted for just a few seconds. People stared at him quizzically and then moved on. They were used to far greater disturbances than a round of applause. How do you know that this was precisely how this flashback played out?There is a lot that I don’t know about that night, so I limited it to the reasonable details that I could verify. After Diaz told me this story the first time, I asked him to re-tell it to me again. And again. And then some more. I asked him about different details, as well as spoke to other people in his life. I confirmed details like the oxygen tubes hanging down from the walls of the hospital with other sources.
“It’s terrible to think about that,” he later said. “It’s like I was wishing the worst on people in that moment. But it was more in the realm of wanting things to get better. I hoped this would be the tipping point, because I don’t ever want humanity to go through something like this ever again.”
The fact that this crumbling system had endured, in spite of all its failures, seemed to him the cruelest fate. “I was telling everyone, ‘If we hobble out of this, I quit,’” he said. “And now, we’re just hobbling out of this, which is infuriating.”
You craft such vivid scenes, either a flashback like this one or real time narrative that follows Diaz and Sanchez through their day. What reporting and writing approaches do you take when creating or recreating scenes?In the field, I try to soak up as much detail as I can through photos, videos, recordings, notes, and lots of questions (when appropriate) or lots of silence (if there’s something happening). This gives me more details to choose from, as well as the opportunity to notice things later on that I might have missed. All of this material can also be a curse. I find it nearly impossible to make decisions, and spend most of the “writing process” in a drawn-out argument with myself over what I am choosing to include or leave out. How important do you find scenes to narrative nonfiction?I often imagine “a scene” as a long, drawn out back-and-forth with dozens of lines of dialogue, as it is in a film or play. In reality, a “scene” in narrative nonfiction is often just a device: it’s a few lines of dialogue or some snapshot of a commotion that allows you to pivot — say, out of the nutgraf and back into the lives of the subjects. It’s often less about verisimilitude and more about moving the plot forward. I often find this process of condensing reality to be quite sad, actually. Borges’ story “The Aleph,” which, in part, laments the many failures of language to adequately represent the plenitude of reality, seems to me a good metaphor for the slightly tragic and unsatisfying nature of non-fiction writing.
No sooner had Diaz shut the metal door to Station 104 than he heard the familiar ring of a call dropping in over the radio — a two-toned descent, like a drawn-out doorbell. “Ugh,” he sighed. “That sucks.” He and Sanchez had just returned to the station after finally offloading their 88-year-old patient into a bed at Antelope Valley Hospital. It had taken over two hours, and the jolt of excitement he’d felt earlier that afternoon had long since dissipated.
“Man, this was our first time back in 14 hours,” he said. This spare, 80-word scene pulls the reader out of the previous digression to convey the exhaustion and near-despair Diaz is feeling. Was it always this brief or did it shrink during revision?It was always quick. The goal was to get us in and out of the station to show us just how little time EMTs sometimes have in between calls before taking us to the point of the scene, which is the actual emergency call.
Diaz had recently switched to this station in Littlerock, a more rural part of the valley known for its fruit orchards and treacherous highway. He’d been working with a different partner at a busier AMR station in Palmdale when he realized he’d had as much as he could take. Clapping in the hallways at the hospital was one sign. Feeling like every problem was the patient’s fault was another. He’d also begun to ask himself what he called “Maslow’s hierarchy of needs type of questions.” Questions, he said, like, “Will I have enough sleep to not negatively affect my home life? Can I eat? Can I use a restroom?” Earlier, you referenced a girlfriend? Did you talk with her?Yes. His girlfriend, Jessica, who is also a hardworking EMT (and now, a paramedic), was incredibly giving with her time. It was actually from her that I learned just how busy and swamped Mike was and how he picked up his phone at all hours — which prompted me to ask him about it. To the point earlier about secondary sources generating details or reporting leads, these details wouldn’t have been the kind of thing that someone as humble as Mike would even think to share with a reporter or had even really noticed about himself. In my outline for the story, I had included a scene of the two of them sitting down for dinner at 9:30 p.m. I loved their exchange — it was about his passion for the union, their relationship in the pandemic, and how he always picked up the phone, even when they were out on a date. But I ultimately chose not to write it into the first draft since it echoed some of the details I had already conveyed through the biographical section. I was also keen to avoid the story including too many conversations since my aim was to keep the story action-driven. Though the Palmdale station was a five-minute drive from his house, his agitation signaled to him that it was time to relocate to what he’d hoped would be a less relentless outpost. So far, though, his new base had been just as hectic as the old one. The recycling bin overflowed with emptied energy drinks. By the time you met him, was he on a more even keel?Mike is always on an even keel. That’s why what he called his brief “hysterical spree” caught him by surprise.
Sanchez, who had just slumped into one of the station’s La-Z-Boys, rezipped her heavy black boots and trudged over to the receiver. “Can you repeat the precaution?” she asked the dispatcher.
Diaz wriggled into the jacket of his uniform and unfastened the Motorola beeper on his hip. “Possibly COVID?” he read from the green band of screen. “Another COVID-positive. Chest pain, 50-year-old man, elevated heart rate with difficulty breathing.” “Green band of screen” is another one of your inventive images that makes the prose so lively. Where did it come from?I saw it. It’s not the sort of detail that I would know existed over the phone.
When Diaz and Sanchez arrived at the address at 8:10 p.m., the road was completely dark, except for the flashing lights on the fire trucks that had showed up moments before them. (Los Angeles County sends both the fire department and an AMR crew to each call.) The patient lived in a converted garage in one of the Valley’s less developed neighborhoods, where the low-slung houses were surrounded by desolate stretches of high desert scrub. It was a crowded home, the kind that Diaz had noticed Latino immigrants often shared with several relatives, making social distancing impossible.
A few minutes later, Diaz and Sanchez slid a coughing man into the back of their ambulance as five family members huddled to wave goodbye. Diaz pressed his boot against the gas pedal and told the dispatcher that they were heading to Palmdale Regional.
What he didn’t say was that he was hurtling toward an overcrowded emergency room with someone who, in his opinion, didn’t need to go there. It’s not that his patient wasn’t sick: The coronavirus had left the man short of breath and, as Diaz drove, he could hear a succession of quick, dry coughs from a few feet behind him. Still, he didn’t think the hospital would be able to do much. The patient was far from needing a ventilator, and with his blood oxygen saturation around 95%, he wasn’t eligible for a nasal cannula under the current rationing orders. It was evident to Diaz that what this man needed was to stay put and rest. But by the time Diaz and Sanchez had entered the patient’s home, the fire department paramedics were finishing up the paperwork to prepare him for transport.
The situation was exasperating. At the scene, the daughter had explained that her father had already gone to the hospital three times in the previous two days and they kept sending him home. Was it really a good idea to bring him back? Whenever possible, Diaz tried to warn patients that unless they were at imminent risk of death — and if he had time to issue this warning, they likely were not — the hospital might not treat them for hours, even days. Still, it wasn’t up to him. EMTs typically handle transport, but the fire department holds the primary medical authority at each call. Again and again, Diaz had seen them abide by a “you call, we haul” mindset. Whose phrase about the fire department’s unwritten policy is that?It was common slang. Diaz used it, along with other EMTs. (Dr. Clayton Kazan, the medical director for the LA County Fire Department, said he understands why EMTs and paramedics “are frustrated that they sometimes have to transport people who seem like they really don’t need to go to the hospital.” But the decision ultimately rests with patients, he noted, and “some of the people who EMTs think don’t have to go to hospital really do end up needing to be there.”)
The knobbly silhouettes of Joshua trees, lit up by the ambulance’s headlights, scrolled by outside the windows. How do you come up with fresh verbs, like “scrolled?”I had seen it in a short story and stored it away. When they approached Palmdale, the arid landscape gave way to a warren of sand-colored strip malls. On rides like this, Diaz wondered, was he helping people feel better or just helping an inefficient system capitalize on people’s fears? The majority of people who call 911 do so for non-life-threatening reasons. Nevertheless, EMTs and paramedics have two options at each scene: leave the patient where they are or take them to the ER — and companies can only charge patients when they do the latter. A recent study of the 911 system by the medical directors of the LAFD noted that this business model “creates a perverse incentive in low-acuity cases (and pandemics) to take all patients to a high-cost, inefficient site” — the hospital — “where one might have to wait hours to be seen and possibly even be exposed to others who are sicker.”
What happened at the hospital was just what Diaz had expected, just as he had experienced it many times before. Because the patient did not meet the county’s new criteria for active monitoring on the wall, Diaz plopped him into a wheelchair and rolled him into the COVID-19-positive section of the waiting room. A scrum of people in pajamas sat on the other side of a plastic curtain. It was the same outcome as if a family member had driven him there. Except for the cost. What was the cost and who pays it?Like the rest of the American healthcare system, it depends on if you have insurance. In Los Angeles County, the bill can run upwards of $1,000 depending on the journey and the resources consumed along the way. Overnight calls and oxygen use cost extra. But ambulance services are usually under-reimbursed, if at all. Much of their clientele — who are poor, uninsured, or both — can’t afford to pay. And even when the government reimburses companies through Medicaid or Medicare, it pays only a fraction of the bill. In California, Medical pays around $120 per ride. I should also note that by law California’s ambulances transport people regardless of their insurance status or ability to pay.
Diaz had nine more hours to go, and he could already feel the stirrings of burnout returning: the irritation, the exhaustion, the apathy. But “burnout” didn’t capture the extent of his distress. It was as if, Diaz said, he was shrouded by a fog. Was he telling you this in real time?We talked about how he was feeling about whatever was happening each day. This frame of mind was something that came up over the course of several interviews. Or maybe it was the other way around, and the fog had lifted, revealing things as they really were. It reminded him of being at a crowded concert and trying to push past a tangle of bodies toward the exit, only to realize that there was no exit. There wasn’t even a door. What happened to Diaz and Sanchez? Did they stay on the job as EMTs?Yes. Things have slowed down considerably. They will be negotiating their contract again this fall.
A few days later, in early February, Diaz and Sanchez were lying in their sleeping bags in the station’s makeshift bedroom area, where five mattresses were pushed up along the walls. Cases had started to decline, and that evening, there’d been a lull in calls. It was one of the first moments they’d had to talk about what had happened to them during the surge. Here you break from the day-in-the-life structure. Did you consider ending the story after the previous paragraph?I didn’t. As many experts have noted, the trauma from the winter is only beginning to surface, and it’s not clear what that “psychological pandemic” will look or feel like. I wanted to move beyond retrospectively chronicling the surge to linger in that future uncertainty. It was important to show that caregivers are just starting to come to grips with what they’ve been through, along with what they did and didn’t allow themselves to feel about it. I also wanted to sit with the fact that even as EMTs continue on with their work — that endless cycle of call after call after call — they’ve been changed by it. EMTS have finally been able to have some quiet moments of private reckoning, but whether a public reckoning will take place to account for the system’s many failures remains an open question. Will these sacrifices have mattered? What if, as Mike says, we hobble out of this, only to just keep hobbling on, without anything changing? What if everyone forgets about what just happened? And what if that forgetting feels better than remembering?
“I feel like where it really hit me — like, we’re not going to get through this for a long time, no matter how much of an effort we put in — was that night in December when I had just come back from having COVID,” Sanchez said. “Were you there that night?”
Diaz said he wasn’t sure. That might have been a shift he’d swapped to get Christmas off.
“I was still partnered with Kirsten,” Sanchez said. “I remember it was one of the first few shifts after I had come back because I was still needing an inhaler nonstop.” How did you behave when they are talking with each other? Did a question from you spark this exchange? And were you interviewing them or were they just talking between themselves while you observed and recorded what they said?It was just after 11 p.m. I’d been asking some questions, and they’d been talking for a while about the kinds of nights they have that make them wonder why they don’t just find a normal job with normal hours. Then, for 17 minutes, they started talking to each other. I only interrupted once during that time to ask, “What happened next?”
That night, she continued, most of the crews had gotten stuck on the wall at Antelope Valley Hospital. There were six or seven COVID-19 patients waiting outside and they all needed high-flow oxygen. Some of them had the lowest blood oxygen saturations she’d ever seen. On 15 liters of high-flow oxygen, her patient’s saturation was only around 84% or 85%. They’d been tearing through the portable tanks every half hour or so, far more quickly than they could be replaced. At one point, she and a few other EMTs opened the metal doors of the storage unit outside the ambulance entrance to the ER and saw that only four tanks of oxygen remained. The charge nurse had already told them that whatever was in there was all that was left, but they knew there were still six patients — or maybe it was seven by now — who each needed a tank to keep breathing. She locked eyes with a colleague, snatched a container for her patient, and hurried away. (A hospital spokesperson said the facility did not run out of oxygen; Wagner acknowledged running low but said AMR is “unaware of any ambulance running out of oxygen.”)
“We were literally watching patients on the verge of coding” — dying — “because there was nothing we could do,” Sanchez said. Although she often thought about this night, she never knew how many of the patients survived. Like many EMTs, she hated to ask the nurses afterward. It was a self-protective measure: out of sight, out of mind.
By the time she picked up another patient, an elderly man, later that night, she’d gone and grabbed one last portable tank of oxygen from the ambulance station. The man’s saturation was around 70%, and she could hear the rales in his breathing. It was a bubbling noise, like the sound of air blown through a straw in a glass of water. After the tank ran out, she tried to console him: “I’m sorry there’s nothing I can do. You just have to wait a little longer.” But he couldn’t understand her. For three hours, he kept repeating the only word he knew in English: “Please.”
“That was the point where I’m literally in the hallway just looking around,” Sanchez went on. “And everywhere you looked it was a disaster. You have the line of patients out the door, still being checked in. And then you hear the frickin’ alarms going off because the hospital is out of oxygen. And the nurses running around. I mean, they’re always running around, but you could tell they’re on a whole other level of overwhelmed.”
“Yeah,” Diaz nodded.
“It’s crazy because you look at your patient and any other day this patient would be a priority, you know? But it’s just that everyone else is in the same scenario. You couldn’t even say, ‘Oh shit, I’m going to panic.’ You just kind of—”
“—shut it out,” Diaz interjected. “It was weird.”
“Yeah, you’re just watching it happen,” Sanchez said, her voice quiet.
“It’s almost existential,” he said. “Like a disconnected, third-person experience.”
Why did you spend so much time on Sanchez’s recollections?Her tale was by far the most nightmarish story I’d heard over the course of my reporting. I couldn’t get it out of my head. And I hadn’t heard or read about anything like it anywhere else. It was like the pandemic’s variation of the Trolley Problem. To confirm its details, I interviewed five other EMTs who were also present that night as well as reviewed text messages sent that evening.
Diaz shifted in his sleeping bag. “I remember there was this weird day in like mid-December where I went on this hysterical spree,” he said, recalling the evening at Palmdale hospital when he’d briefly hoped for the worst. “I started thinking this was all funny, and that the whole system just needed to collapse. I’m almost mad that it’s started tapering off. How can we go to this edge and it doesn’t collapse? People are going to forget about it in a year, and we’re going to be right back to the same place where our system still sucks.”
Sanchez tried not to think about the future. Until now, she hadn’t had the time to focus on anything other than the immediate needs of patients.
“Usually after you have a bad call, like one with a kid, you can cry if you need to and process those feelings,” she said. “But I feel like I never addressed that part of it with these types of calls. I’m sure it’s building up.”
“It’ll probably result in some PTSD later or something,” Diaz said, laughing.
Sanchez smiled sardonically. “Yeah, but that’s not today’s issue.”
“That’s how it is, and that’s very EMS, that way of thinking about things,” he said. “Like, ‘Don’t worry about something until you have to worry about it.’ It’s almost in our training: ‘Don’t get too ahead of yourself, because doing that will not allow you to be in the moment to help other people.’ So it’s, like, ingrained in us to—” What recording technology were you using?Just a pocket-sized Sony. I use my iPhone as a backup. I put them in different locations in whatever room I’m in, even if it’s just on different sides of my chair, since one will often pick up bits of audio and sound that the other might miss.
As Diaz spoke, the pager on his hip began to vibrate. Then the loudspeaker chimed.
Another call.
They sat up, pulled on their boots, and walked back to their ambulance.
The ending is terrific, concluding the story with a moment of understated pathos about the plight of these anonymous foot soldiers of the pandemic. Out of all the moments you observed, how did you settle on this for the ending?It was ironic — or, at least, it was telling for me — that just as Mike was talking about staying in the moment, another call arrived. Even when he is trying to process the nature of this work — its relentless ongoingness — he has no choice but to keep going. Heading back into the field to heed yet another call seemed like an ending, but it also seemed like a sort of beginning.
About this story:Ava Kofman spent three weeks reporting in person with EMTs in Los Angeles for this article. She either witnessed the scenes described here or gathered the details, including participants’ thoughts at the time, from interviews with those participants. Why was the note about your reporting methods appended to the story? I wonder if such an explanation should be available to readers at the top so they understand things like how you were able to write about Diaz’s thoughts before they read the story?This was something that ProPublica found useful. I’m less persuaded that it’s necessary, actually, since these standard reporting techniques have been widely practiced since the New Journalism of the 60s and 70s (and long before). I hope a note like this never appears at the top of anyone’s story; it seems like it would distract from the story itself and possibly be misread as some sort of demerit, addendum, or correction.
***
Chip Scanlan is an award-winning journalist who spent 15 years teaching at The Poynter Institute. He now writes and coaches writers from his home in St Petersburg, Florida, and publishes Chip's Writing Lessons,



