When ProPublica health policy reporter Lizzie Presser tackles a new national story, she follows the dictum of essayist E.B. White: “Don’t write about Man; write about a man.” So when she and her editor, Alexandra Zayas, wondered if using one disease “as a lens into problems in our health care system” might be be illuminating, “I wanted to find a condition that was pervasive, preventable, and potentially deadly,” she said. She chose diabetes, which afflicts more than 34 millions. While many carefully manage it for a lifetime, it can too easily lead to coma, blindness, nerve damage, kidney failure, limb loss and, of course, death.
Eventually, Presser found her way to diabetes-plagued rural Mississippi, and the man whose story would carry a narrative 7,200-word narrative about the fate of Black diabetes patients at the mercy of a medical and insurance complex that is behind a 50 percent increase in amputation rates. That despite vast strides in medicine and technologies that make amputation a questionable decision. Worse, she told me, “Black Americans were three times more likely than all other Americans to suffer amputations.’
The protagonist of “The Black American Amputation Epidemic” is cardiologist Dr. Foluso Fakorede, a larger than life Nigerian-raised doctor who settled in Bolivar County, Mississippi, and has mounted what Presser describes as a “militaristic” campaign to stem the tide of amputations among Black patients. Billboards dot the countryside with Fakorede’s message: Amputation Prevention Institute.
Presser weaves the cardiologist’s campaign and personal story with a penetrating investigative strain, buttressed by damning sections and embedded with links to scientific studies that document how racial biases in the medical and insurance communities deny Black Americans the kind of care that he provides.

This isn’t an untold story, “In my view, the reality is more grim,” Presser, said. Medical studies about racial disparities in amputations have been reported for decades — but have received little attention from politicians or journalists. Presser’s story pushes back at that shortcoming.
Her reporting is empathetic and indefatigable — she met with upwards of 60 patients — infusing the writing with both authority and concern. Her research was wide and deep: She read medical studies, histories of the region, and even a local poet whose work helped her describe the sweet smell of the Delta soil.
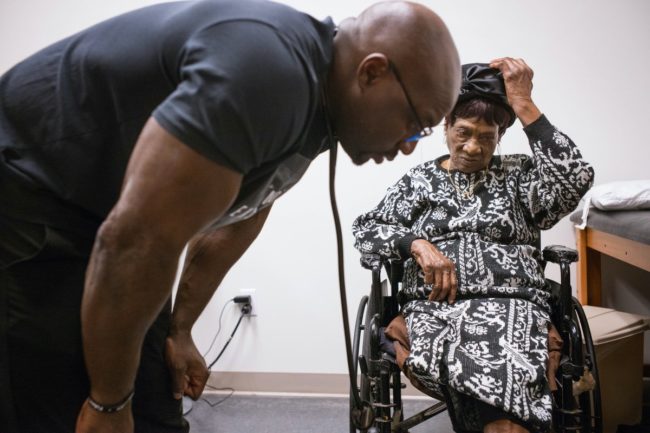
When Fakorede didn’t respond to her calls and letters, she traveled to the county and successfully made her case to shadow him in his practice. For a month she followed him into patient’s rooms, with their permission, and then interviewed them at their homes. While Presser documented gruesome and heartbreaking cases, she also noted some successes: An older man, Henry Dotstry, already lost one leg to diabetes, but Fakorede offers hope for the remaining limb.
Dramatic scenes propel Presser’s story — but so does her own outrage at what she witnessed. I asked how she felt when she learned that Black diabetes patients were denied crucial angiograms that could detect blocked leg arteries, her answer was a single word: “Livid.”
The amputation investigation was packaged with “Tethered to the Machine,” which tracks a Black man on dialysis as he fights to get on a kidney transplant waiting list in Alabama. Standing in his way: similar tragic barriers faced by Fakorede’s patients. Together, the stories won the 2021 National Magazine Award for public interest.
Before joining ProPublica, Presser’s work appeared in The California Sunday Magazine, The New Yorker, The Guardian, This American Life and others. Her story “The Dispossessed,” published in partnership with The New Yorker, won the George Polk Award for Magazine Reporting and the John Bartlow Martin Award for Public Interest Magazine Journalism in 2020. She is a two-time finalist for the Livingston and the National Magazine awards.
Nieman Storyboard spoke with Presser about her research and verification methods, her approach to structure and writing investigative narratives, and the variety of ways she shed light on a neglected story. Our conversation has been edited for length and clarity, and is followed by an annotation of the text.
The Black Amputation Epidemic appears to be an untold story, at least in the general press. How did you discover it?
When I was asked to take on a health beat in 2020, my editor Alexandra Zayas and I wondered if it might be illuminating to use one disease as a lens into problems in our healthcare system. I wanted to find a condition that was pervasive, preventable, and potentially deadly. I quickly zeroed in on diabetes, and started digging into the complications.
I was startled to see that despite the great strides in diabetes medicines and technologies, the rate of amputations had increased by 50% between 2010 and 2015. And I was appalled by the disparities: Black Americans were three times more likely than all other Americans to suffer amputations.
How did you find Dr. Fakorede?
When I’m writing a national piece, I try to ground the narrative in a local story. My hope was that if I reported in a county where amputations were particularly prevalent, I’d be able to get a clearer sense of what was driving amputation rates, how the amputations were experienced, and how doctors, hospitals and policymakers could address the unnecessary surgeries. Mississippi and South Carolina had some of the highest rates, and as I dug into what advocates and physicians were saying in those states, I found a short blog post by Dr. Fakorede, a limb-salvage specialist in the Mississippi Delta. He wrote about addressing unnecessary amputations as a moral imperative, and I could sense his anger and determination in his prose. I started calling him and writing to him with no luck. I got on a plane to Jackson, Mississippi, to meet other limb-salvage specialists and patients, but after several days of reporting, I still couldn’t quite see the story. I drove out to Dr. Fakorede’s office to introduce myself in person, and he finally agreed to speak with me. After a few hours talking about his path to this work, I realized that I could write a story about him, his practice, and his patients. And once he understood that I didn’t want to write a quick-turn piece — that I wanted to shadow him for a month to see what he sees — he got on board.
At the same time, you document the resistance of the medical and insurance communities to endorse limb-saving treatments. Would you detail the reporting that led to these damning conclusions?
It wasn’t until I got on the ground and started hearing patients tell their stories that I really understood how hospital decision-making, fee-for-service payments, and insurers were contributing to the amputation epidemic. Dr. Fakorede had his own opinions about the resistance he saw, and I watched in real-time as many of the obstacles he had explained to me played out among his patients in need of care. It was quite striking.
What was your goal for this story?
At some level, I wanted to make readers feel as outraged as Dr. Fakorede did. And then I also wanted to unravel several complex factors that were driving the rise in amputations and the great disparities in care. I chose to look most closely at three issues: a task force that hadn’t recommended screenings for at-risk patients; the federal government’s choice not to forgive the student loans of specialists who focus on treating diabetic complications in remote areas, and policy gaps around limb-saving procedures before an amputation.
The story deftly braids Dr. Fakorede’s campaign targeting specific cases with the larger issues that undermine the care of Black Americans. Tell us how you approach structure in a case like that?
I wasn’t sure how I was going to structure this story for some time. I figured that Dr. Fakorede’s professional arc could help showcase how much work it takes to prevent diabetic amputations, and I was meeting with patients whose stories I thought I could unspool if I didn’t find an urgent case while I was there. I met Henry Dotstry on my final weekend in Mississippi, and I immediately knew I wanted to follow his story. Dr. Fakorede was so angry about the care Henry wasn’t getting, and it was the first time he was open with me about the specific obstacles he was up against at the hospital. It was also the first case where I could observe everything that Dr. Fakorede needed to do in order to provide his patient with an opportunity to keep his leg. At the same time, I could track the emotional upheaval for Henry and his family.
Once I was set on these two main subjects for the story, I outlined a few different woven structures until I landed on the one that felt the most fluid.
This story, with its reflection of a tragic human situation and an indictment of the system that enables it, is both powerful and seamless. Could you unpack your writing process?
I think that observation extends to the way Dr. Fakorede saw his work: He understands this epidemic as an indictment of our healthcare system, and he had spent years parsing out the various causes before I knocked on his door. I say this to explain that I find that, often, any power I’m able to summon in my writing is usually a result of the reflections of the people I get to write about.
…any power I’m able to summon in my writing is usually a result of the reflections of the people I get to write about.
As for the actual writing, I am a devoted outliner at the start. For this story, I printed out hundreds of pages of interviews and transcribed scenes and tried to read through them within 24 hours so the material was fresh in my mind. I usually outline on a computer, but in this case, there was so much that I wanted to use that I started cutting up paragraphs and quotes and details and laying them out on the floor. This is the most difficult and the most exciting part of the process for me. I’m trying to craft a narrative with suspense at the same time as I’m trying to construct a logical argument. Once I’d laid out my outline on the floor, I left it there for weeks as I tried to write through it. I would move pieces around on the floor to see how changes would play. And as I was writing, I was trying to keep the voices of my subjects in my head. I wanted my prose to reflect how they thought and spoke.
Are there literary or journalistic influences you draw on for stories that combine investigative reporting and narrative nonfiction? Did you draw on any particular models as you reported and wrote your story?
I re-read my favorites regularly, like Katherine Boo, whose subjects are always such lively company, Rachel Aviv, whose psychological lens I adore, and Linda Villarosa, whose insightful work on public health I deeply admire. But this was a new form for me, relying heavily on observed scene. I knew I needed to let my reporting dictate the form.
What role did your editors play in the process?
My editor, Alexandra Zayas, helped nail down some of the details of the structure. I doubted that we could pull away from Henry’s story for two full sections before diving back into his care, but she showed me how we could. She’s got the best accountability eye I know, and she also pushed me early on to think through the breaks in the system that got us to this place. Plus, once the words are on the page, she really knows how to amp up the drama.
Annotation: Storyboard’s questions are in red; Presser’s responses in blue. To read the story without annotations, click the ‘Hide all annotations’ button, which you’ll find just below the social media buttons in the top right-hand menu or the individual gray boxes throughout the text, or at the top of your mobile device.)
The Black American Amputation Epidemic
by Lizzie PresserMay 19, 2020
IT WAS A FRIDAY EVENING in the hospital after a particularly grueling week when Dr. Foluso Fakorede, the only cardiologist in Bolivar County, Mississippi, walked into Room 336. Henry Dotstry lay on a cot, his gray curls puffed on a pillow. Fakorede smelled the circumstances — a rancid whiff, like dead mice. He asked a nurse to undress the wound on Dotstry’s left foot, then slipped on nitrile gloves to examine the damage. Dotstry’s calf had swelled to nearly the size of his thigh. The tops of his toes were dark; his sole was yellow, oozing. Fakorede’s gut clenched. Fuck, he thought. It’s rotten.
You launch the narrative with a detailed and gruesome scene that takes the reader into middle of the action of a medical emergency. But you balance the misery with the touching image of Dostry’s “gray curls puffed on a pillow.” How and why did you decide to open your narrative this way?During a month of reporting, this was the moment that made Fakorede the most angry. I wanted to start in medias res because that’s how Fakorede’s most pressing work often begins: in the midst of a potential tragedy -- an amputation. The clock is usually ticking, and he needs to figure out if and how he can prevent a surgery. I also wanted the camera to introduce our two lead subjects here: the physician and his patient.
Who identified the rancid smell as “dead mice?” You?I heard another doctor use this term and I thought it captured the smell perfectly.
How do you know that’s what went through Dr. Fakorede's mind?I interviewed him immediately after this occurred. I pushed him to walk me through every step and each thought he could remember. Of course, you never know if people are telling you the truth. But by this point, I’d spent so much time with him that I could detect what felt most authentic.Many publications refuse to publish profanity, instead leaving out letters for words like “Fuck.” Why does ProPublica allow its use? Thank god they do! It’s a great word. Fakorede rolled his eyes when I told him I’d described his nausea as his “gut clenching.” But he knew the “Fuck, it’s rotten,” sounded like him.
Fakorede, who’d been asked to consult on the case, peeled off his gloves and read over Dotstry’s chart: He was 67, never smoked. His ultrasound results showed that the circulation in his legs was poor. Uncontrolled diabetes, it seemed, had constricted the blood flow to his foot, and without it, the infection would not heal. A surgeon had typed up his recommendation. It began: “Mr. Dotstry has limited options.” Do you consider this foreshadowing?I thought of it more as a way to show the stakes.
Fakorede scanned the room. He has quick, piercing eyes, a shaved head and, at 38, the frame of an amateur bodybuilder. Dotstry was still. His mouth arched downward, and faint eyebrows sat high above his lids, giving him a look of disbelief. Next to his cot stood a flesh-colored prosthetic, balancing in a black sneaker. How and why did you choose the case of Henry Dotstry as the character whose story dominates the narrative, woven in through multiple encounters with Dr. Fakorede. Were you presented with other cases that you decided against using in this key role?Before I met Henry, I’d been meeting with patients who had already suffered amputations or narrowly avoided them, and I was reporting out their stories and reconstructing what they’d experienced. Once I met Henry and his family and learned how quickly Fakorede needed to act to save Henry’s leg, I realized I was finally witnessing what Fakorede had tried to explain to me in interviews. Readers could watch along with me as I observed the time-pressured nature of this work, and I could document the findings through observation.
“How’d you lose that other leg?” Fakorede asked. Dotstry was tired, and a stroke had slowed his recall. Diabetes had recently taken his right leg, below the knee. An amputation of his left would leave him in a wheelchair. Given Dotstry’s impairment, how did you learn about his medical history and prognosis? And given patient privacy laws, how were you able to confirm it?I heard about Dotstry’s medical history pretty quickly, and his siblings and niece filled in some of the gaps. Henry also allowed me to request his medical records so we could fact-check dates and diagnoses.
Fakorede explained that he wasn’t the kind of doctor who cuts. He was there because he could test circulation, get blood flowing, try to prevent any amputation that wasn’t necessary. He hated that doctors hadn’t screened Dotstry earlier — when he’d had the stroke or lost his leg. “Your legs are twins,” he said. “What happens in one happens in the other.”Why did you paraphrase what Dr. Fakorede said at the start of the paragraph and then punctuate it with a quote?I loved the idea of our legs being twins, and it was a line that had stuck with me, helping me understand some of the failures of preventive care in these cases. If an artery in your left log is clogged, it’s likely that an artery in your right leg will become clogged, as well. No one had told Henry this, so he wasn’t getting proper preventive care to keep his other leg healthy. I try to stick to quotes that show us something about the person who is speaking, and in this case, I also liked that this was how Fakorede made medical information really easy to understand.
Dotstry needed an immediate angiogram, an imaging test that would show blockages in his arteries. He also needed a revascularization procedure to clean them out, with a thin catheter that shaves plaque and tiny balloons to widen blood vessels. Describing medical procedures, cutting through jargon, is often difficult, yet you do so clearly that the reader can envision and understand the treatment Dotstry needs. Who described it to you? And did you ask a medical professional to review the description for accuracy?My high school biology teacher, Dr. Church, would tell you that I have long been fascinated by how the body works. There’s a lot of room to play with language, and I try to do so as clearly as I can because I trust that most of us want to know better what the hell is happening inside of us. For these paragraphs, I kept trying to find language that was accurate and also visually compelling. By the end of this story, I was running all of my descriptions of medical procedures and disease processes by three different specialists who could tell me if I had erred from the facts. They didn’t always agree with one another, so it was a tricky dance.
His foot was decaying, fast. Though Fakorede ran an outpatient practice nearby, when doctors consulted him on inpatients at Bolivar Medical Center, the local hospital, he expected to use its facilities.
He asked his nurse to schedule the procedures. But by the time he had driven home to his ranch house on the northern edge of town, he hadn’t received an answer. Nor had he when he woke up on Saturday at 3:30 a.m., as he did every morning. By sunrise, he was restless at his kitchen counter, texting the hospital’s radiology director, explaining the need for an intervention on Monday, Martin Luther King Jr. Day. Within a few hours, he got a response: “I don’t have the staff or the supplies. I’m sorry.”
Now Fakorede was mad, walking briskly into his office, dialing friends on speaker phone, pacing around his conference room.
How much of the previous passage reflects live reporting or narrative reconstruction?I wondered if you’d ask this question. I wasn’t there on the Friday that Fakorede met Dotstry. I didn’t have permission from the hospital to shadow Fakorede. I was, however, at his house interviewing his parents, and when he came home that evening, he started ranting about what he’d just seen. I interviewed him almost immediately, and then I drove back to his house the next morning around sunrise, when he was trying to figure out what to do. I was a witness on Saturday.When you do reconstruct a scene, how do you collect the details and verify them? It depends on the circumstances, but I try to gather as much detail as I can from everyone who was there. Often I tell subjects that I want to get to a place where I can close my eyes and see it like a movie, but with more sensual detail: smell, touch, taste. In this instance, I could walk through the consultation with Dr. Fakorede and ask, “and what did you say?” “and what did you think?” “and then what happened?” “and you said you put on gloves, but what kind of gloves did you put on?” All the very slow “can you walk me through it?” questions. Luckily, it was still fresh in his memory. When I went to the hospital the next day, I could observe the room — how Henry looked, the smell of his wound — and I would bring those details back to Dr. Fakorede, or structure questions with those details in mind. It’s the tiniest observations that will give a story the texture I want.
He’d been raised in Nigeria, moved to New Jersey as a teenager and had come to practice in Mississippi five years earlier. He’d grown obsessed with legs, infuriated by the toll of amputations on African Americans. His billboards on Highway 61, running up the Delta, announced his ambitions: “Amputation Prevention Institute.” You pack a lot of information in this 51-word paragraph. Did it emerge in one draft or require revisionOh, this took several rounds of revisions. This is, in some ways, our introduction to Fakorede, and I wanted to convey a few quick thoughts: He’s an outsider, he’s obsessed, and this is a problem so large that the man has erected billboards.
Nobody knew it in January, but within months, the new coronavirus would sweep the United States, killing tens of thousands of people, a disproportionately high number of them black and diabetic. They were at a disadvantage, put at risk by an array of factors, from unequal health care access to racist biases to cuts in public health funding. These elements have long driven disparities, particularly across the South. One of the clearest ways to see them is by tracking who suffers diabetic amputations, which are, by one measure, the most preventable surgery in the country. What enabled you to reach these conclusions?Many were already well established in public health literature. The racial disparities in COVID-19-related deaths were still new and unfolding, but the early research was quite clear. I was particularly drawn to the idea of diabetic amputations as a symbol: Here is what some researchers refer to as the most preventable surgery in the country, and what we learn from the failures to reduce amputations holds lessons for the financing and structuring of our healthcare system more broadly.
Look closely enough, and those seemingly intractable barriers are made up of crucial decisions, which layer onto one another: A panel of experts decides not to endorse screening for vascular disease in the legs; so the law allows insurance providers not to cover the tests. The federal government forgives the student loans of some doctors in underserved areas, but not certain specialists; so the physicians most critical to treating diabetic complications are in short supply. Policies written by hospitals, insurers and the government don’t require surgeons to consider limb-saving options before applying a blade; amputations increase, particularly among the poor.
Despite the great scientific strides in diabetes care, the rate of amputations across the country grew by 50% between 2009 and 2015. Diabetics undergo 130,000 amputations each year, often in low-income and underinsured neighborhoods. Black patients lose limbs at a rate triple that of others. It is the cardinal sin of the American health system in a single surgery: save on preventive care, pay big on the backend, and let the chronically sick and underprivileged feel the extreme consequences. This strikes me as a nut graf, a powerfully crafted and authoritative passage summing up the infuriating cycle that leads to a tragic result. How much reporting and thinking went into it, and what gave you the confidence to lay it out without attribution?I don’t know how to quantify how much reporting and thinking went into it. I wrote a pretty clunky nut graph to get it out of the way in my first draft, but I was also spending a lot of time speaking with my editor about what the story was really about. It was those conversations, and the work we did together untangling it all, that allowed me to see the obstacles as layers that I needed to peel back for the reader.
Fakorede grabbed his car keys and headed to the hospital. He walked straight to the lab. As he suspected, it had all the supplies that he needed. Why won’t they give me staff? he wondered. They wouldn’t do that to a surgeon. Why did you use italics here, as you did in the first paragraph that reveals his thoughts?In this section, I’m setting up Dr. Fakorede as our guide. Instead of quotes or reflections that he says to me, I want you, the reader, to feel like you’re following him through this maze.
He has little tolerance for this kind of transgression. He is militaristic, to an extreme.Why do you call him that?I wanted to give the reader a sense of the guy and this was an economical way to do so. He suits up in camouflage vests for his procedures and says things like, “Ready for war?” He had spoken to me at length about how the military boarding school he had attended as a kid had shaped his work ethic.
To him, nonhealing wounds are like heart attacks. “Time is muscle,” he repeats. He calls huddles when nurses forget to check a patient’s ankles: “If you haven’t assessed both legs, I don’t want to walk into that room.”
He considers each of his procedures an act of war.
When people stand in his way, he sends a barrage of text messages, punctuated by exclamation marks. And he uses his cellphone to collect evidence that the system is working against his patients, and his efforts.
He pulled out his iPhone and photographed the hospital’s wires and catheters, IVs and port protectors.. He shot the images over to the hospital’s radiology director. Fakorede’s private practice was closed for the holiday weekend. He calculated that he had only a few days to carry out some plan before Dotstry’s remaining leg was amputated.
TWO MAPS EXPLAIN why Fakorede has stayed in the Mississippi Delta. One shows America’s amputations from vascular disease. The second shows the enslaved population before the Civil War; he saw it at a plantation museum and was stunned by how closely they tracked. On his phone, he pulls up the images, showing doctors, or history buffs, or anyone who will listen. “Look familiar?” he asks, toggling between the maps. He watches the realization set in that amputations are a form of racial oppression, dating back to slavery.
Fakorede was initially tempted to move to the Delta while practicing in Tennessee. He befriended a medical device sales rep named Maurice Hampton who had grown up in the Mississippi region. Hampton talked about how black families were leery of local hospitals and how few black doctors in the Delta specialized in vascular work. “It’s the norm to go to Walmart and see an amputation or a permacath in the neck,” he’d told Fakorede. Why didn’t you define "permacath" here for readers?I didn’t want to distract from our main focus.
“If you don’t see one, then you didn’t stay but two minutes.”
Then, a little over a year into his Tennessee job, Fakorede found himself at loose ends. He’d raised concerns that he was being billed for expenses that weren’t his and asked for an audit; though the audit later found that the clinic where he worked had claimed over $314,000 in improper expenses, he was quickly terminated. Fakorede sued the clinic for retaliation under the False Claims Act and lost.
(The clinic’s lawyer said his client had no comment, but there were “numerous” reasons for Fakorede’s departure.) In the spring of 2015, he had a mortgage, a quarter of a million dollars in student debt and four months of severance pay. He also had an impulse to understand the Delta.
Your story gets inside Dr. Fakorede’s head and also tracks his actions as he fights against a systemic medical and insurance denial of care for these cases. How much time did you spend with him and in what settings? Did it take time for him to open up to you?I spent a lot of time with him. I’d say about six hours a day, six days a week, for four weeks. He’s an extroverted man, so he was open with me quite quickly, but it took time for him to get comfortable reflecting on himself. I joked about that with him a fair amount. And slowly, some of his walls started to come down.
Fakorede spent four days driving through its long, flat stretches of farmland dotted with small towns and shotgun houses. The wood-slat homes and bumpy roads reminded him of his grandparents’ village in the Nigerian state of Ondo, where he’d spent summers as a kid. He drove scores of miles on the Mississippi highways without seeing a single grocery store; fast-food chains lit the busiest intersections. He was startled by the markers of disease — the missing limbs and rolling wheelchairs, the hand-built plywood ramps with metal rails. He thought of amputees like “an hourglass,” he said, “that was turned the day they had their amputation.” Did you drive around the Delta to verify the description of what he saw?Oh yeah. I drove around a whole lot, took notes, and kept my eyes out for visual cues. I mentioned the plywood ramps to him, and he remembered being struck by them too.
Mortality rates rise after the surgeries, in part, because many stop walking. Exercise improves circulation and controls blood sugar and weight. The less activity a person does, the higher the risk of heart attacks and strokes. Within five years, these patients were likely to be dead.
Fakorede weighed taking a lucrative job up north, near his parents, who had both been diagnosed with diabetes. He had professional connections there; he’d gone to Rutgers Robert Wood Johnson Medical School and done a residency at New York-Presbyterian Weill Cornell Medical Center. But the South, he felt, needed him. About 30 million people in America had diabetes, and Mississippi had some of the highest rates. The vast majority had Type 2; their bodies resisted insulin or their pancreas didn’t produce enough, making their blood sugar levels rise. Genetics played a role in the condition, but so did obesity and nutrition access: high-fat meals, sugary foods and not enough fiber, along with little exercise. Poverty can double the odds of developing diabetes, and it also dictates the chances of an amputation. One major study mapped diabetic amputations across California, and it found that the lowest-income neighborhoods had amputation rates 10 times higher than the richest. The Delta was Mississippi’s poorest region, with the worst health outcomes. Fakorede had spent years studying health disparities: African Americans develop chronic diseases a decade earlier than their white counterparts; they are twice as likely to die from diabetes; they live, on average, three years fewer. In the Delta, Fakorede could treat patients who looked like him; he could find only one other black interventional cardiologist in the entire state. A growing body of evidence had shown how racial biases throughout the medical system meant worse results for African Americans. And he knew the research — black patients were more responsive to, and more trustful of, black doctors. He decided after his trip that he’d start a temporary practice in Mississippi, and he rented an apartment deep in the Delta.The story is studded with online links that support many of your descriptions and conclusions about the epidemic. How do you decide when to use them?We decided to link to these studies in the spirit of public service. If a doctor or a patient or a curious reader wanted to learn more, she could follow the trail of blue. Some of this research preceded my time in Mississippi, and some came after, when I was fact-checking or conducting follow-up on interviews.
He fantasized about building a cardiovascular institute and recruiting a multidisciplinary team, from electrophysiologists to podiatrists. But as he researched what it would take, he found a major barrier. Medical specialists with student debt, who graduate owing a median of $200,000, generally could not benefit from federal loan forgiveness programs unless they got jobs at nonprofit or public facilities. Only a few types of private practice providers — primary care, dentists, psychiatrists — qualified for national loan forgiveness.
The Delta needed many other physicians. Though Bolivar County was at the center of a diabetes epidemic, there wasn’t a single diabetes specialist, an endocrinologist, within 100 miles.How did you verify this? Does ProPublica have a specific fact-checking process?I asked a few other referring doctors in the Delta if this was their experience, too. I also used data from the American Association of Clinical Endocrinology to map the endocrinologists in the region. We don’t usually work with fact-checkers at ProPublica.
Fakorede leased a windowless space in the Cleveland Medical Mall, a former shopping center that had been converted to doctors’ offices. People came to him with heart complaints, but he also asked them to remove their socks. Their legs alarmed him. Their toes were black and their pulses weak. Their calves were cold and hairless. Some had wounds but didn’t know it; diabetes had numbed their feet. Many had been misdiagnosed with arthritis or gout, but when Fakorede tested them, he found peripheral artery disease, in which clogged arteries in the legs limit the flow of blood.
This is what uncontrolled diabetes does to your body: Without enough insulin, or when your cells can’t use it properly, sugar courses through your bloodstream. Plaque builds up faster in your vessels’ walls, slowing the blood moving to your eyes and ankles and toes. Blindness can follow, or dead tissue.How did you learn enough to summarize the cascading effects of diabetes with authority on your own, rather than quoting experts or studies?I read a lot. I spoke to diabetes specialists. And I learned a ton while shadowing Dr. Fakorede, as he explained to patients what they were experiencing and then broke it down further for his nurses and assistants.
Many can’t feel the pain of blood-starved limbs; the condition destroys nerves. If arteries close in the neck, it can cause a stroke. If they close in the heart, a heart attack. And if they close in the legs, gangrene.
Within a month, Bolivar Medical Center had credentialed Fakorede, allowing him to consult on cases and do procedures in the hospital. His most complicated patients came in through the emergency room. Some arrived without any inkling that they had gangrene. One had maggots burrowing in sores. Another showed up after noticing his dog eating the dead flesh off the tips of his toes. Fakorede took a photo to add to his collection. “It was a public health crisis,” he told me. “And no one was talking about amputations and the fact that what was happening was criminal.” The details here are revolting. Did you have any problems being exposed to such graphic misery? I did not enjoy seeing the photographs, and in this passage, I wanted to convey the level of horror I felt.
On weekends, Fakorede had been driving back to his five-bedroom home in Tennessee, but in August of 2015, he decided to go all-in on Bolivar County.
He sold his house and black Mercedes G-Wagon, and applied for funding to build a practice in the Delta: Cardiovascular Solutions of Central Mississippi. He pitched himself as a heart guy and a plumber, removing buildup in the arteries. Four banks denied him loans, so he borrowed money from friends. He gave himself a two-year window to reduce amputations and publish his outcomes.
THE DELTA FLOOD PLAIN runs 7,000 square miles along the northwestern edge of the state, with sweet-smelling, clay-like soil cordoned between bluffs and the banks of the Mississippi River.Smell is an underused sensory detail in stories? Where'd this specific reference come from?I spent a lot of time reading about land in the Delta. I wanted to transport readers there, and many of the patients I was meeting had grown up working in the fields. That history was part of this story. It was the local poet and planter William Alexander Percy who described the soil as “sweet-smelling,” and I loved it.
By the 19th century, the primeval forests had been transformed into a cotton empire; at the start of the Civil War, more than 80% of people in many Delta counties were enslaved. Sharecropping emerged after emancipation, and black farmers cultivated small plots in return for a portion of their crop. They lived on credit — for food and feed and clothing — until the harvest, but even then, their earnings rarely covered their expenses.
For decades, African Americans in the South struggled to find and afford health care. The American Medical Association excluded black doctors, as did its constituent societies. Some hospitals admitted black patients through back doors and housed them in hot, crowded basements. Many required them to bring their own sheets and spoons, or even nurses. Before federal law mandated emergency services for all, hospitals regularly turned away African Americans, some in their final moments of life. What were your sources for this historical context?I read a great book titled “Out in the Rural,” by the historian Thomas J. Ward Jr., which details the fight for one of the first Federally Qualified Health Centers in the country, right here in Bolivar County. I followed many of the footnotes in that book to other sources. And I scoured academic journals for papers on the history of racism in the AMA and the growth of black-owned hospitals.
Fakorede was drawn to Bolivar County, in part, because of its history. He’d run out of gas there when he was first scouting the region, and later that evening, he’d Googled its background. For a brief moment, Bolivar was the center of a movement for public health care, driven by the conviction that racial equality was not possible without justice in health. In 1964, when a group of physician activists traveled to the Delta, Robert Smith, a black doctor from Jackson, saw rocketing rates of intestinal parasites and maternal death. “I understood for the first time what it truly meant to be black in Mississippi,” he told a magazine. Under President Lyndon B. Johnson’s War on Poverty, a Boston doctor secured funding to open a community health center in Bolivar, which he grew with the help of Smith. Clinicians worked with residents to take on housing, sanitation, exercise and nutrition. Its success spawned a national project of more than a thousand Federally Qualified Health Centers for the underserved. But funding shrank under President Richard Nixon, and the centers’ initiatives were scaled back to basic primary care.And how did you learn about this? Whenever I’m traveling to a new city or county, I read up on its history. There was so much about Bolivar that I wanted to include, but I ended up focusing on its role as the birthplace of community health centers because of the significance in a story about unequal access to care. Any time I am writing a piece that’s looking at potential solutions to a problem, I’m equally interested in the choices that created that problem in the first place. I try to weave in this history as much as I can throughout.
By the time Fakorede moved to the Delta, in 2015, the state had the nation’s lowest number of physicians per capita. It had not expanded Medicaid to include the working poor. Across the country, 15% of African Americans were still uninsured, compared with 9% of white Americans. That year, Jennifer Smith, a professor at Florida A&M University College of Law, wrote in the National Lawyers Guild Review what Fakorede saw firsthand: “While the roots of unequal and inequitable health care for African Americans date back to the days of slavery, the modern mechanisms of discrimination in health care has shifted from legally sanctioned segregation to inferior or non-existent medical facilities due to market forces.”Why did you use this specific reference?I thought her writing drove home that these disparities in care did not arise in a vacuum. Even if the American healthcare system today adheres to anti-discrimination law, it continues to deprive Black Americans of equal access to quality care.
Fakorede understood that to reach patients, he needed referrals, so he met primary care providers at hospitals and clinics. He asked them to screen for vascular disease, measuring blood pressure at the ankle and the arm. Many didn’t have the time; given the shortage of local physicians, some were seeing up to 70 patients a day. If my math is correct, in a 14-hour day that means just 12-minute appointments? Did you verify this number? I asked several primary care physicians to tell me their caseloads. I also went to the doctor a few times with different patients and timed how long the doctor stayed in the room.
Others didn’t know much about peripheral artery disease or why it was important to diagnose. Some were offended by Fakorede’s requests. Michael Montesi, a family doctor, was grateful for the help, but he found it brash for the new doctor in town to start telling the veterans what to do. He recalled thinking, “Where were you the first 12 years of my practice, when I needed a cardiologist, when I needed an OB-GYN, when I needed a surgeon, when I had to do an amputation in the ER, or deliver a baby that was 23 weeks and watch the baby die because there was nobody there that could take care of him?”How did you conduct the interview with Montesi?We were actually all eating dinner -- Dr. Fakorede, Dr. Montesi, and I. At this point, I’m not sure if Dr. Fakorede was listening or not, but I had my recorder on. I try to meet people in person if I’m in town. I find it far more comfortable than if we’re on the phone.
The brushoffs disturbed Fakorede, but when he dug deeper, he realized that the doctors weren’t only overwhelmed; they had no guaranteed payment for this vascular screening. The Affordable Care Act mandates that insurers cover all primary care screenings that are recommended by the U.S. Preventive Services Task Force, an independent panel of preventive care experts. The group, though, had not recommended testing anybody without symptoms, even the people most likely to develop vascular disease — older adults with diabetes, for example, or smokers. (Up to 50% of people who have the disease are believed to be asymptomatic.) As specialists, cardiologists are reimbursed if they screen patients with risk factors. But by the time patients got to Fakorede, the disease was sometimes too far along to treat. Many already had a nonhealing wound, what’s known as “end stage” peripheral artery disease, the last step before an amputation.
How did you decide when in the narrative to pull back from the closeup of Dr. Fakorede and his patients to the larger issues that explain and underscore the causes of the Black amputation epidemic?In some ways, this is a question about rhythm. I’m structuring this story around small moments of suspense. At the same time, I’m attempting to show what details consumed and enraged Fakorede. If I can get you to see, perhaps even feel, Fakorede’s anger as he tries to save Dotstry’s leg, I’m more likely to keep you reading. I’ve set up the story with a “will he or won’t he” frame, which becomes one driving force of suspense. In this passage, I want you to see that he’s not simply fighting against a single for-profit hospital, but he’s up against a national task force that guides the country’s insurance policies. I’m planting that Fakorede has more work to do beyond saving this patient’s leg. Will he take that on, too?
When Luvenia Stokes came to Fakorede, she had already lost her right leg at the age of 48.
Like many Delta residents, she grew up in a food desert, and without money for fresh produce, she’d developed diabetes at a young age. She said that a pedicurist nicked her toe, and the small cut developed an infection. Without good blood flow, it began bubbling with pus. Stokes told Fakorede that no doctor had performed an angiogram to get a good look at the circulation or a revascularization to clean out the arteries. A surgeon removed her second toe. Without cleared vessels, though, the infection spread. Within weeks, a new surgeon removed her leg.Why did you introduce additional patients?I wanted the reader to see the scope in an article that is describing the great number of people suffering from unnecessary surgeries. As a reader, I appreciate when a story leaves me with small images, so I try to give the same to anyone reading me, like Luvenia’s toe that’s nicked during a pedicure.
Stokes lived in a single-wide trailer with her mother. Her wheelchair could not fit in the doorways, so she inched through sideways with a walker.How did you find and interview Ms. Stokes?I met her through Dr. Fakorede. Then I visited with her before she had a follow-up appointment with him. I drove out to her trailer early one morning. We chatted as she ironed her hair and her mom smoked cigars.
Because she could hardly exercise, she gained 48 pounds in two years. The amputation hadn’t treated her vascular disease, and a stabbing pain soon engulfed her remaining leg, “like something is clawing down on you,” she said. When she finally made it to Fakorede, she told him that one doctor had prescribed neuropathy medication and another had diagnosed her with arthritis. “I’m not letting them get that other leg,” Fakorede told her. Stokes’ grandmother, Annie, who lives in a nearby trailer, had lost both her legs, above the knee, to diabetes. Her cousin Elmore had lost his right leg, too.
General surgeons have a financial incentive to amputate; they don’t get paid to operate if they recommend saving a limb. And many hospitals don’t direct doctors to order angiograms, the most reliable imaging to show if and precisely where blood flow is blocked, giving the clearest picture of whether an amputation is necessary and how much needs to be cut. How do you know this?I couldn’t find a single hospital that did direct doctors to order angiograms because hospitals generally leave the practice of medicine to the physicians. I hedged by saying “many.” Insurers don’t require the imaging, either. (A spokesperson for America’s Health Insurance Plans, a leading industry trade association, said, “This is not an area where there is likely to be unnecessary surgery.”) To Fakorede, this was like removing a woman’s breast after she felt a lump, without first ordering a mammogram.
Nationwide, more than half of patients do not get an angiogram before amputation; in the Delta, Fakorede found that the vast majority of the amputees he treated had never had one. Now, he was determined to make sure that no one else lost a limb before getting the test. This wasn’t a controversial view: The professional guidelines for vascular specialists — both surgeons and cardiologists — recommend imaging of the arteries before cutting, though many surgeons argue that in emergencies, noninvasive tests like ultrasounds are enough. Marie Gerhard-Herman, an associate professor of medicine at Harvard Medical School and a cardiologist at Brigham and Women’s Hospital, chaired the committee on guidelines for the American College of Cardiology and the American Heart Association. She told me that angiography before amputation “was a view that some of us thought was so obvious that it didn’t need to be stated.” She added: “But then I saw that there were pockets of the country where no one was getting angiograms, and it seemed to be along racial and socioeconomic lines. It made me sick to my stomach.” Why did you inject yourself in the narrative here and in the next paragraph, the first times that you do so? How do you make that decision?For most of this story, Dr. Fakorede is the authority. We are watching him do his job, commenting on the failures of care, trying to fight a system that was never designed to reduce amputations. A medical professional, in my view, was a more trustworthy expert than I could ever be. In this section, I’m signaling to the reader that I’m here, too, and I am also doing my due diligence on Dr. Fakorede and all that he is advocating for. As the author of this story, I promise I won’t let you get fooled. How did you find Dr. Gerhard-Herman?She wrote the guidelines for cardiologists. I wanted to go to a leader in Dr. Fakorede’s field, and she seemed like just the right fit.
Stokes wasn’t at immediate risk of losing her left leg when she met Fakorede, but pain prevented her from walking. She had a severe form of the disease, and Fakorede booked her for an angiogram and revascularization. He inserted a wire into her arteries and cleaned out the clogged vessels, letting oxygen-rich blood rush to her remaining foot. While she was recovering in Fakorede’s lab, she thought about her neighbors who had the same problems. “I really don’t like what’s happening to us,” she said to me. “They’re not doing the tests on us to see if they can save us. They’re just cutting us off.”
Patients didn’t know about vascular disease, or why their legs throbbed or their feet blackened, so Fakorede went to church. The sales rep, Hampton, introduced him to pastors, and several times each month, he stood before a pulpit. He told the crowds that what was happening was an injustice, that they didn’t need to accept it. He told them to get screened, and if any surgeon wanted to cut off their limbs, to get a second opinion. In the lofty Pilgrim Rest Baptist Church, in Greenville, he asked the congregation, “How many of you know someone or know of someone who’s had an amputation?” Almost everyone raised their hands. Were you at the church that day?I was not, but one of Fakorede’s employees had filmed this, so I watched the video.
At first, Fakorede took a confrontational approach with colleagues. Some seemed skeptical that he could “prevent” amputations; it’s a tall claim for a complex condition. Once, when a doctor had disregarded his advice, he’d logged it in the electronic health record, so the oversight would be on display for anyone who looked up his patient’s chart. Fakorede could fume when people questioned his authority; self-confidence carried him, but it sometimes blinded him to his missteps. Over time, though, Fakorede tried to rein in the arrogance. “You peel off a layer that may be comprised of: I’m from up North, I know it all, you should be thankful we’re here to provide services that you probably wouldn’t get before.” He picked up some Southern manners. Fakorede began texting doctors with photos of their patients’ feet along with X-rays of their arteries, before his intervention and afterward. Referrals picked up, and within a year, he’d seen more than 500 patients.
But Bolivar Medical Center, he learned, was turning away people who couldn’t pay a portion of their revascularization bill upfront. Several former employees told me the same. How did you find employees who would talk? Did you have to grant them anonymity?It’s a small town. If I think a piece of information could cost someone a job, and I don’t think it’s necessary to identify them, I won’t identify them. In this case, I put this question directly to the hospital as well, and they chose not to respond to it. If they had said it wasn’t true, I would have gotten this allegation on the record.
“It’s a for-profit hospital, it’s no secret, it’s the name of the game,” Fakorede said. “But a for-profit hospital is the only game in town in one of the most underserved areas. So what happens when a patient comes in and can’t afford a procedure that’s limb salvage? They eventually lose their limbs. They’ll present back to the emergency room with a rotten foot.” And a surgeon would have no choice but to amputate. (A hospital spokeswoman said that last year, it gave $25 million in charity care, uncompensated care and uninsured discounts. Asked if it turned away patients who couldn’t pay for revascularization, she did not respond directly: “We are dedicated to providing care to all people regardless of their ability to pay.”)
The practice was discriminatory, he reasoned, and also financially backward. At $237 billion in medical costs each year, diabetes is the most expensive chronic disease in the country; one of every four health care dollars is spent on a person with the condition. Left untreated, the costs pile on. Medicare spends more than $54,000 a year for an amputee, including follow-ups, wound care and hospitalizations; the government program is the country’s largest payer. Then come the uncounted tolls: lost jobs, a dependence on disability checks, relatives who sacrifice wages to help with cooking and bathing and driving.
By the time Carolyn Williams came to see Fakorede, in 2016, she’d been uninsured with diabetes for 20 years; she’d worked at a housing nonprofit and for a food assistance program, but neither had offered coverage. At the age of 36, she’d needed a triple bypass surgery, and at 44, she had three toes amputated. Untreated leg pain left her needing a wheelchair; she pulled out of Delta State University, where she was pursuing a degree in social work. Fakorede reconstituted blood flow in her legs and got her walking. But the diabetes was already destroying her kidneys. She joined the government’s disability rolls. She also went on dialysis, at a yearly cost to Medicare of $90,000. Did you interview Ms. Williams? I met Ms. Williams through Dr. Fakorede, and I spent a lot of time with her. I wanted to keep this description short, though, because it wasn’t necessarily moving the story along. It punctuates the piece with an example of how twisted the system is. I didn’t see a need to add a quote.
On the days when Fakorede wanted to give up and leave, he drove to an Emmett Till memorial in Money, Mississippi. After 14-year-old Till was mutilated and murdered, in 1955, his mother had insisted on opening his casket. “Let the people see what I’ve seen,” she said, and his image brought national outrage to racist violence in the South. Fakorede thought often about how that decision sparked the Civil Rights movement. He thought about it as he exhibited his photos of rotten feet and limbless bodies, his own proof of what he considered a modern atrocity. He didn’t want to live by Bolivar Medical’s policies. He decided that in order to treat as many people as possible, irrespective of income or insurance, he needed to build a lab of his own.
THIS JANUARY, THAT LAB was now Dotstry’s best shot. The hospital’s consulting surgeon expected to amputate his leg below the knee. He had written that because Dotstry’s kidneys were impaired, the contrast dye in an angiogram would be dangerous. But Fakorede could replace the dye with a colorless gas, which wouldn’t jeopardize Dotstry’s health.
It would have made the most sense to perform the procedure at the hospital; Dotstry had been admitted and was occupying a bed. But after Fakorede opened his outpatient lab and hired away two techs and a nurse, a spokeswoman said the hospital stopped doing certain interventions. She told me it shouldn’t have surprised Fakorede that they couldn’t schedule Dotstry’s case, and that if he had been unable to treat a patient in his lab, the hospital could have worked with him to find another. Fakorede told me he’d never received such a message. When a doctor asks him to treat an inpatient with an acute condition, his responsibility, as he sees it, is to do it in the hospital. “If I don’t have a hospital that wants to coordinate,” he asked, “what do I do?”
The answer, at least this time, was to get his patient out of there. He called Dotstry’s doctor and convinced her to discharge him for the intervention. Then, at noon on Saturday, Fakorede walked back into Room 336. Given that you were there on Friday when Dr. Fakorede examined Mr. Dotstry’s legs and it’s Saturday now, were you in the room when he arrived or were you traveling with him?I was in the room. I had already met Dotstry’s family, so I asked his sister if I could go with her to the hospital. I had been re-reading Eli Saslow’s work in The Washington Post, and I loved when he made it seem like he was operating two cameras at once: one that follows a person into a scene or out of a scene, and another that follows the scene. I wanted to be in Dotstry’s room so I could facilitate a similar switch: keep one camera on Fakorede, while leaving another focused on the family.
Dotstry’s sister, Judy, was standing by his bed. She wore tall leather boots over acid-washed jeans, with a thick, black wig in a braid down her back. You present the reader with striking descriptions of your characters. I notice that often follow the rule of threes, using three specific, informed details that influences pacing or allows the reader to visualize a character or situation.I find that drawing out two details sometimes feels anemic, and four can be overwhelming. That being said, three can feel formulaic. I find physical description quite hard.
Fakorede handed over his card. “I called the hospital to see if we can do this case on Monday,” he said, “and they said no.”
Judy inhaled. “What now?”
Fakorede laid out the plan for a Monday morning angiogram in his own procedure room. He would open up as many vessels as he could. If he could get circulation to Dotstry’s foot, he might be able to save it. He wasn’t sure about the toes. Given HIPAA regulations that protect patient privacy, how were you able to gain access to patients and their families in the hospital and Fakorede’s lab? Fakorede and his nurses and I set up a system at his practice. I would shadow Fakorede in the halls, and when he or his nurses went to check on patients in private rooms, they would ask the patients if they felt comfortable with a journalist attending. If they did agree to be in the story, we would also ask them to sign release forms. I was lucky to find a doctor who was willing to work with me to make this happen. I didn’t have the same access at the hospital, so I only went there as a guest of patients I had already met.How many of his patients did you see in all?I easily met over 60 of Dr. Fakorede’s patients.
When Dotstry had suffered his stroke several years back, Judy had become his caregiver. She’d stopped taking jobs in home care and supported her brother without pay — shuttling him to doctors’ appointments, controlling his sugars, managing his medications. After his amputation, she’d helped him learn to walk again. In place of a salary, she’d drawn disability for an old work injury; she’d been electrocuted while operating a machine, and the nerves in her arm were damaged, making her hands tremble. But she couldn’t stay unemployed forever. This past fall, she had gone back to work, cleaning the local post office.
After Fakorede left, Judy looked over at her brother, who sat slumped over the side of the cot, a blue gown slipping off his bony shoulders. Their father had been a sharecropper, and Dotstry had dropped out of elementary school to help on the farm, harvesting soybeans, rice and cotton. Of 10 kids, he was the oldest boy, and he took care of the others, bringing in cash and cooking them dinner. They almost never saw a doctor. Instead, they’d relied on cod liver oil, or tea from hog hoofs, parched over a fire.
Dotstry had spent his career driving tractors, hauling crops and plowing fields, but he wasn’t insured and still rarely saw doctors. At 60, when he was diagnosed with Type 2 and prescribed insulin, he didn’t know how to manage the medicine properly; he had never learned to read. Insulin pumps were too expensive — more than $6,000. His blood sugar levels often dropped, and he sometimes passed out or fell on the job. Little by little, his employer cut back his duties. In 2015, he had a stroke; diabetes had raised his risk. A year later, his right foot blackened and was amputated at the ankle. The infection kept spreading, and soon, his lower leg went. He could no longer work.
Two of his sisters had died after complications of diabetes. Judy had stood over their beds like she was now standing over Dotstry’s. He’s still here, she reminded herself.
She pulled out her phone and called another brother. “They gonna amputate his foot, cause it’s bad,” she said. “Toe’s rotted.”
Dotstry looked up from the bed. “No!” he shouted. “They can’t take that off. Why?”
“Why you think your foot look like that? Why you think it smells? It stinks!” she said. Dotstry reached down to unwind the gauze. Judy wondered why he hadn’t told her that his foot was infected sooner. She lowered her voice. “You were doing pretty good. If you wasn’t, I could have tried to get back in there and do something.” This is such haunting dialogue. Were you taking notes or using an audio recorder, and if so, what kind?I was pretty stunned to be in the room for this whole exchange. I kept a small Sony audio recorder running the whole time, and I took as many notes as I could on the blocking: where and how people were composing themselves in the room, their expressions, their silent actions.
Her daughter, Shequita, ran into the room, huffing. She was loud and pissed off. Why did you use “pissed off” and not “angry?”It was her term.
“Whose foot is that?” she shrieked. She kneeled by the cot and helped Dotstry scoot up onto his pillow, stretching out his legs. He was usually a prankster, a hard-headed contrarian, the uncle who’d picked her up and spun her around like an airplane. She was thrown off by how quiet he’d become. In the passage above, you use third person to convey Shequita’s views of her uncle. Why not quote her?I wanted to stay in the moment here. These were the thoughts running through her mind. To stay in the present, I needed to write them as such, rather than as later reflections, which would mean jumping around in time.
“Your daughter wants to know if you want to come stay with her, if you want to come to Texas,” Shequita told him.
Dotstry knew the offer was on the table, but he hadn’t yet accepted. A few days earlier, a tornado had torn the roof from his trailer, and he was, for the moment, without a home.
“She said it’s a lot better doctors up there,” Shequita continued, “and if she gotta stop working to take care of you, she can do that.” She gripped her hands around the frame of the bed and leaned over it, locking her eyes with his. “I need you to be thinking hard about this, sir. This ain’t you. I need you to get back to you.”
“He ain’t gotta go to Texas,” Judy interrupted.
Shequita shot back: “You gonna take care of him?”I’m struck by the way people act so naturally in your presence.I was also surprised that Judy, Shequita, and Henry were comfortable with me being there. This was such a tense moment for the family that I don’t think they were considering me at all. I said nothing during the scene I recount here. I sat in a chair with my recorder on and took visual notes.
Judy was silent. She knew that she couldn’t, not like before. She needed her paycheck for home repairs; a flood had warped her wooden floors. But Dotstry’s daughter was younger, and Judy thought that if she quit her job at Walmart, she’d get restless. Besides, Dotstry knew no one in Texas. She pictured him in a wheelchair, staring off, confused about where he was. Judy figured if he went, he’d go on and die.
She crossed her arms. “He’ll be all right if they don’t have to amputate that leg,” she said.
Shequita looked at her mother. She walked over to where she stood, by a shaded window, and threw her arms around her neck. Then, she left the room. Judy hoisted herself up onto the foot of her brother’s cot. She swung her legs up so that she faced him, and she laid herself down. What a poignant scene. Did you know when you witnessed that it belonged in the story? Immediately. My pulse was racing through this entire exchange, and when I left the hospital that afternoon, I knew this scene would be a climax in the story, if only because it had such a strong hold over me. I was overcome by the urgency in the room, and I wanted readers to feel that, too.
ABOUT EVERY FIVE YEARS, the doctors and researchers who make up the U.S. Preventive Services Task Force reassess their screening guidelines. In 2018, the members returned to peripheral artery disease and the blood flow tests that Fakorede had asked local primary care doctors to conduct. Once again, the panel declined to endorse them, saying there was not enough evidence that the tests benefited the average asymptomatic American.
In their statement, they acknowledged that public commenters had raised concerns that the disease “is disproportionately higher among racial/ethnic minorities and low-socioeconomic populations” and that this recommendation “could perpetuate disparities in treatment and outcomes.” In response, the panel said it needed better evidence. But as the National Institutes of Health has found, minorities in America make up less than 10% of patients in clinical trials.
Dr. Joshua Beckman, the director of vascular medicine at Vanderbilt University Medical Center, was an expert reviewer of the evidence base for the task force, and its final report struck him as irresponsible. It hardly noted the advantages of treatment after screening; the benefits were right there in the data that he saw. The panel discounted the strongest study, a randomized control trial, which demonstrated that vascular screening, for men ages 65 to 74, reduced mortality and hospital days. (The study bundled peripheral artery disease screening with two other tests, but in Beckman’s eyes, the outcomes remained significant.) He was confused about why the task force had published its evaluation of screening the general public, when it was clear that the condition affects specific populations. Several American and European professional society guidelines recommended screening people with a higher risk. “You wouldn’t test a 25-year-old for breast cancer,” he told me. “Screening is targeted for the group of women who are likely to get it.”
Dr. Alex Krist, the chair of the task force, repeated the group’s position in an email that the data was not strong enough to endorse screening, even for at-risk patients. “The Task Force does not do its own research, so we can’t fix these research gaps, but we can — and did — ring the alarm bell to raise awareness of this vital issue among researchers and funders.”Why did you quote from an email rather than an interview?Dr. Krist didn’t want to talk on the phone so, regrettably, I didn’t have a choice.
Vascular surgeons who have spent their careers studying limb salvage have come to see preventive care as perhaps more important than their own last-ditch efforts to open blood vessels. Dr. Philip Goodney, a vascular surgeon and researcher at Dartmouth and White River Junction VA Medical Center, made a name for himself with research that showed how the regions of the country with the lowest levels of revascularization, like the Delta, also had the highest rates of amputation. But revascularizations aren’t silver bullets; patients still must manage their health to keep vessels open. Now, Goodney believes his energy is better spent studying preventive measures earlier in the disease’s progression, like blood sugar testing, foot checks and vascular screening. Many patients have mild or moderate disease, and they can be treated with medicine, counseled to quit nicotine, exercise and watch their diet. “We need to build a health system that supports people when they are at risk, when they are doing better and when they can keep the risk from coming back,” he told me. “And where there’s a hot spot, that’s where we need to focus.” Tell me about finding and using Goodney here.He’s the preeminent researcher on the issue. Most researchers cited his work, and when I started looking into the mapping he had done, I reached out to him. Luckily, Dr. Goodney was also willing to work with us on our own visualization. My very talented colleague Lena Groeger took the lead on this, and once she got Dr. Goodney’s underlying data, she built the maps that we used in the story. How likely is it that patients with diabetes, especially in low-trust areas, would follow this kind of advice?Well, the advice isn’t nearly as effective as it would be if it came with resources. What Goodney is saying, though, is that we need a health system that accounts for this.
Fakorede scrolled through the task force’s statement. “You want more data? Really? Who has the highest amputation rates in America?” he asked. “That’s your data.”
He had taken to the national stage, speaking at conferences about what he’d witnessed in Bolivar. On behalf of the Association of Black Cardiologists, he testified before Congress, convincing U.S. Rep. Donald M. Payne Jr., a Democrat from New Jersey, along with U.S. Rep. Gus Bilirakis, a Republican from Florida, to start a Congressional Peripheral Artery Disease Caucus. The group is pushing for the task force to reevaluate the evidence on screening at-risk patients, for federal insurers to start an amputation prevention program and for Medicare to ensure that no amputation is allowed before evaluating arteries. Other groups are advocating for legislation that would require hospitals to publicly report their amputation rates. Why did you decide to make Fakorede’s mission the through line of your story, blending it in with the overall picture of the systemic problem? My colleague Ava Kofman recently told me that she is often looking for a protagonist who is pushing many boulders up a mountain. I think that’s an apt description of what I’m looking for, too, particularly when the focus of a story is on a person who is trying to effect change. When I first got to Mississippi, I kept meeting with individual patients, but I realized quite quickly that I couldn’t tell this story well enough through one person’s story. I’m describing a phenomenon with immense scope, and I wanted to convey that breadth. In Fakorede, I found a physician who had committed his life to taking this on. He was determined to provide better care for his local patients despite the obstacles he faced; he wanted government resources for specialists like himself who worked in under-resourced hotspots; and he was pushing for national legislation that would create clear screening guidelines for at-risk patients and would ensure that patients receive an evaluation of their arteries before an amputation.
In Bolivar, Fakorede had seen more than 10,000 cardiovascular patients from around the Delta. How did you verify this number?His nurse kept a record.
Dr. DeGail Hadley, a primary care provider in town, told me that before Fakorede arrived, he wasn’t sure what was best to do for patients with rotting feet. “It was always a process of transferring the patients to Jackson or Memphis, which can be difficult.” Both cities were two hours away. Now, Fakorede was performing about 500 angiograms annually in town. Last year, he published a paper in Cath Lab Digest describing an 88% decrease in major amputations at Bolivar Medical Center, from 56 to seven. (Fakorede did not provide me with all of his sources.) Did this cause you to doubt his case? I didn’t doubt his case. And once the hospital came back with its figure of a 75% reduction, I certainly felt comfortable. Fakorede couldn’t find the underlying data on the first year of amputations — the 56 figure. I wrote to the journal and to other co-authors, and they couldn’t find it either. I was unsettled by that. I wanted the reader to know I wasn’t taking Dr. Fakorede at his word and that I wasn’t able to fully fact-check his findings.
The hospital has different internal figures, which also reflect a significant decrease. Between 2014 and 2017, the hospital recorded that major amputations had fallen 75% — from 24 to six.
Fakorede couldn’t catch everyone in time, and he was haunted by the patients who got to him too late. A week before he’d met Dotstry, Sandra Wade had come in with an open sore on her right big toe. She came from a family of diabetics. Her mother had died after a diabetic coma. Her cousin had just lost a leg. Her oldest sister, who’d raised her, had given up on walking when a tired, burning, itching sensation consumed her legs. Now, Wade felt it, too.
“I don’t want to give up like that,” Wade had said, reclining in a cot in Fakorede’s pre-procedure room. “I want my toes. I don’t want to lose not one limb. I choose life.” She elongated her O’s. She was 55 and had a high, gentle voice, a wide smile and big, curled lashes under loose, curled hair. She had spent most of her career in food service and retail, recently managing a Family Dollar, but after diabetes took her eyesight, she’d had to quit. She wondered if the sodas and chips that had fueled her at the store had accelerated her disease. Or if she’d focused so much on her son, who was developmentally disabled, that she’d neglected herself. She didn’t like to offload blame onto her genes. “Somebody’s gotta try to change the cycle,” she’d said. “I really want to be the one.”
Fakorede inserted an IV into the top of her leg. He opened up each of her blocked arteries, one at a time, until he got to the most important one, which ran along her inner calf. It was supposed to supply blood to her open wound, and she needed it to heal. Without it, she’d likely lose her toe. If she didn’t control her sugars, she could lose her lower leg next. Fakorede was hopeful as he slid a wire through the vessel in her knee, and into that crucial artery in her calf. But then, about a third of the way down, it stopped. It was as if the vessel itself had evaporated. What’s the implication of this development involving the artery along her inner calf? You are not the first person to ask this question, which means I didn’t do my job well enough here. If Fakorede can’t get all the way through the vessel with a tiny wire, then there’s no way that blood, and the nutrients that blood carries, can get through; it’s unlikely that her wound is going to heal, and it’s likely that she’ll lose her toe.
UNDER A CRISP, WIDE SKY, on Martin Luther King Jr. Day, churches around town were opening their doors for services. Fakorede’s office was scheduled to be closed, but he’d called in his nurses and radiology technicians, even those out hunting deer, to staff Dotstry’s case.
“What’s up, young man?” Fakorede greeted Dotstry, who was slowly fading into his Ambien, and he handed Judy a diagram of a leg. “The prayer is that we can find this many vessels to open up,” he said, pointing to the paper. “As soon as I’m done, I’ll let you know what I find.”
In the procedure room, he put on his camouflage-patterned lead apron, and with an assistant, Why didn’t you identify his assistant or nurses?I think too many names can distract a reader. I wanted to keep the plot moving. he inserted an IV near Dotstry’s waist. He wound a wire across Dotstry’s iliac artery, into the top of his left leg. The femoral artery was open, even though it had hardened around the edges, a common complication of diabetes. They shot a gas down the arteries in Dotstry’s lower leg so the X-ray could capture its flow. Fakorede looped his thumbs into the top of his vest, waiting for the image. Other than a small obstruction, circulation to the toes was good. “They don’t need to whack off the knee,” he said, staring at the screen. Dotstry would lose one toe.
After they’d cleaned out the plaque, Fakorede called Judy into the lab and pulled up the X-rays. Dotstry snored in the background. The doctor showed Judy a playback of the blood moving through the vessels. She could tell that his foot had enough flow. She folded over, running her palms along her thighs. “Y’all have done a miracle, Jesus.”
Dotstry would need aggressive wound care, help controlling his sugars and a month in rehab following his toe amputation. In the meantime, Judy and her daughter would have to learn to manage his antibiotics and find him an apartment. He’d still be able to tinker with his cars, as he did most afternoons. And as far as Judy was concerned, he wasn’t moving to Texas.
Fakorede scrubbed out. He sat at his desk to update Dotstry’s doctors. He called an infectious disease specialist, 35 miles south, to check on whether he could see Dotstry the following morning. Then, he dialed the hospital and asked for one of the nurses. He explained what he’d found: that Dotstry didn’t need a leg amputation.
“Oh, great,” the nurse replied. “The surgeon was calling and asking about that. He called and tried to schedule one.”
Fakorede had been typing up notes at the same time, but now he stopped. “He was trying to schedule it when?” he asked.
“He was trying to schedule it today.” How did you get both sides of the conversation? To protect my sources, I unfortunately can’t disclose this.What a resonant ending. When you heard it, did you know you had your ending for the story? Did you continue reporting afterwards?I knew this would be the ending, or at the very least, the near ending. After several weeks with Dr. Fakorede, this was the first time that I had seen with my own eyes that he could prevent an amputation. I did keep reporting, though. I went with Dotstry to his follow-up appointments to track if his wound could heal, and it could. I also needed to corroborate the course of events with the surgeon who had scheduled his amputation.
***
ABOUT THE REPORTING
For this story, Lizzie Presser spent over a month in Mississippi, in December and January, speaking with dozens of patients and shadowing doctors, in clinic and in procedures. She interviewed over a dozen medical professionals whose work has intersected with Fakorede’s, including nurses, limb-salvage specialists, primary care providers and the hospital’s consulting surgeon, Dr. Roger Blake, who corroborated all facts related to his treatment plan for Henry Dotstry. She asked Bolivar Medical Center if it believed it provided Dotstry with adequate care. Even with Dotstry’s permission, the hospital declined to comment on his case, citing patient privacy.
The scenes in the story are informed by her own observations and interviews with the subjects to fill in details, including their thoughts at the time.
To put her observed reporting into national context, she reviewed the salient medical research and interviewed more than a dozen experts in all corners of the health care system, from those who treat diabetic patients to those who inform and set policies around care.The editor’s note is especially detailed. Do you think it’s a good practice to append one?ProPublica is committed to explaining the how of reporting, and I certainly don’t think it hurts to include an editor’s note with this level of detail.
***
Chip Scanlan is an award-winning journalist and former faculty at The Poynter Institute. He lives and writes in St. Petersburg, Florida, and publishes Chip’s Writing Lessons, a newsletter of tips and inspiration.



