Over his career at the Los Angeles Times, Thomas Curwen has written and edited for the Outdoor section, the Book Review, the features desk and the Metro desk. Despite his wide-ranging interests, his enduring passion is for stories that, as he puts it, depict “the split-second events that change the predictable course of life.” That passion paid off in his Pulitzer-winning contribution as part of the team that reported on the San Bernardino terrorist attack, and his Pulitzer finalist work about a grizzly bear attack in Montana.
A story on gun violence, then, would fit nicely with Curwen’s interests. But when he set out to report a story on the ratcheting trend in 2013, on the heels the Sandy Hook massacre, Curwen noticed the market was saturated with pieces that focused on gunmen or the victims. So he found a different main subject: the trauma surgeon.
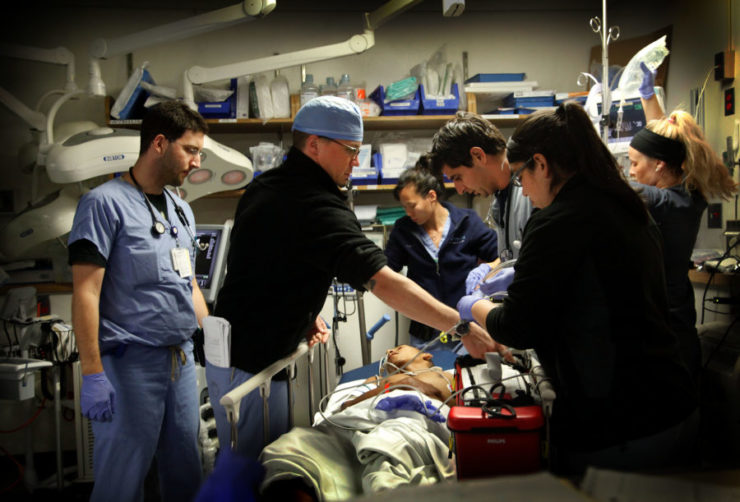
Five months after securing clearance to Harbor-UCLA Medical Center, Curwen and a photographer witnessed, from inside the operating room, as Dr. Brant Putnam raced to save the life of a teenage boy. The resulting story is a pulsating and spare tick-tock of an all-too-common phenomenon in American hospitals.
This interview has been edited and condensed.
You’ve worn a lot of hats at the Times over the years. When you reported this piece, were you on a specific beat? How did you find this story?
Gun violence in America had once again moved to the front page, and most stories, it seemed, focused on the shooters and the dead. I wanted to find a different angle. Two years earlier, I had written about the firefighters and paramedics who arrived on the scene of a similar tragedy at a hair salon in Seal Beach, and I knew that every time a bullet found its victim, it set off a ripple of effect, concentric rings running throughout our society, changing the lives of families, bystanders, medical professionals, even those reading the news.
I wanted to see how surgeons and emergency room personnel cope with these senseless, almost daily shootings, and I began calling local hospitals to see if I might be able to report this story from their perspective.
For you, is this a gun violence story or a trauma surgeon story? Or both? Or neither?
This is the story about a random act of violence that upended the life of the victim and his family, but by focusing on the surgeon who treats gunshot wounds almost every day, I wanted to see if the experience was somehow uneventful. This intrigued me: How can the world collapse at the point of a gun, bringing with it death and tragedy, and leave some unscathed, even undeterred by these events? How do they understand gun violence (and this country’s inability to stop the bloodshed)?
In terms of your final narrative product, it feels spare, or at least as though it could’ve been much longer, with far more context and backstory. Why did you choose to focus the aperture in this way?
After reporting the story, I realized I had a straightforward chronology. I just needed to get the clock running in the most efficient and economical way, introducing the reader to the emergency room and the two main characters: the surgeon and the boy. Beyond that, I wanted to get out of the way, laying out each detail in the most clear and economic manner, avoiding unnecessary detours and medical jargon. When writing action sequences, I find that short sentences are the most effective, staccato bursts of language, that convey speed, franticness and urgency. Longer sentences would have slowed the rhythm of the prose, and these are no moments to linger over. A life was at stake.
Similarly, I felt that too much backstory – those detours – would have distracted the reader. This account had to be as focused and as sharp as possible.
In many ways, this story reminded me of Jon Franklin’s famous piece “Mrs. Kelly’s Monster,” which won the first Pulitzer Prize for feature writing. Are you familiar with that story? Did you take inspiration from that or any other writing when putting this together?
I am flattered by the association, and yes, I am familiar with Franklin’s masterful story. It certainly has become the hallmark for medical narratives, to which I would add Tom Hallman’s “The Boy Behind the Mask.”
As much as I admire these stories, I don’t know if I can say if they influenced me. I read widely, drawing upon a lot of different narrative styles, and in this case, I credit my sources, namely Dr. Putnam. Once I had completed a draft of the story, I met with him, and we talked about our four hours in the operating room, a conversation that allowed me re-report the story and go deeper in the material.
"After reporting the story, I realized I had a straightforward chronology. I just needed to get the clock running in the most efficient and economical way, introducing the reader to the emergency room and the two main characters: the surgeon and the boy. Beyond that, I wanted to get out of the way."
You mentioned to me that one of the most difficult aspects of reporting was getting access to the surgical operation. How did that process work? Did you feel that being in the room while it was happening was essential?
The challenge of reporting any story in a hospital setting is HIPAA (Health Insurance Portability and Accountability Act), which prohibits medical personnel from disclosing information about their patients.
In the past, I’ve secured permission from patients before I began reporting. They would sign a waiver allowing me access to their records and histories.
In this case, however, any individual coming into a hospital with a gunshot wound would not be in any position – physically or mentally – to sign any waiver, let alone understand who I was and what I was attempting to do.
As a result, the photographer on the story – Barbara Davidson – and I were able to work out an arrangement with the hospital and their attorneys to report the story under the condition that once the patient was in recovery, we would explain our intentions. If the patient agreed – and then signed the waiver – we could proceed. If the patient did not agree, we would destroy my notes and images.
It was a gamble, and we were fortunate that Harbor-UCLA Medical Center agreed to these terms. In the end, the hospital staff – and the patient and his family – understood the importance of our work.
The story reads quickly, at times during the surgery almost like an avalanche, an assault on the senses. Was it intentional to create a sweeping energy like that?
It’s a good observation, and yes, that was the intent: to capture the chaos, the uncertainty, the fear and terror of this moment, these seconds that passed as hours on the operating table.
Surgeon races to save a life during L.A.’s shooting season
By Thomas CurwenOriginally published August 18, 2013
From the entry wound — the size of a nickel — Dr. Brant Putnam guesses that the bullet is a .45, but it's what he can't see that worries him most. What went into your decision to start in the hospital, almost inside the head of the surgeon we haven’t met?I am great advocate for telling a story as close to the point of view of the protagonist as possible. This story is Dr. Putnam’s story, and I wanted to establish from the very beginning. All that we’re seeing and experiencing comes from his perspective. Technically, this makes attributions more invisible and creates a more immediate, less intrusive reading experience.
The boy, a teenager most likely, lies naked on Bed 2 in a trauma bay at Harbor-UCLA Medical Center. His brown skin, slick with sweat, is ashen.
"What's your name?" a resident asks as half a dozen doctors and nurses circle him.
The boy can't answer.
"Ohhh," he moans.
"How old are you, sir?"
"Awww."
The boy's hipbones delicately protrude from his narrow waist. He has a woman's name tattooed down his right arm from elbow to wrist and the bullet hole is to the right of his navel. These details are incredibly intimate. What purpose was served by including them here?I wanted to capture the vulnerability of the human body, most obvious when it is stripped naked. The boy’s skinny frame and his tattoo were the canvas of his youth, possibly his innocence, and the bullet hole, the stunning interruption. I also believe that the more intimate the detail, the more universal the appreciation. I didn’t want the reader to be distracted by questions of race which often figure in stories about gun violence. I wanted these hipbones, that right arm, that naval help connect us immediately to this stranger, this boy, just like all of us.
Putnam, chief of trauma, stands back and watches and listens. He is puzzled that the wound is hardly bleeding.
"Sit up for me."
"Ohhh."
There is no sign of an exit wound.
"Hey. Wake up."
A resident slaps the boy. They need him conscious.
Putnam knows the surge of adrenaline that brought the boy this far is nearly spent. If his blood pressure crashes, his heart will stop. Putnam wonders if it is too late.
"Let's go to the OR," he says, loud enough to get everyone's attention.
The season of shootings has begun on time. Were you not worried that this “season of shootings” may need some explaining?It is always a challenge to weave statistics into a narrative, but in this case, they are critical. They explain the urgency of this story and lay out why we are here in the first place. So rather than present the numbers like a news story (107 GSWs in three months), I wanted to set them up with a quick lead-in – alliterative, perhaps disarmingly poetic – with the hope that any confusion would quickly be answered by the consecutive sentences.
Last year, from July through September, this Torrance hospital treated 107 gunshot victims, the highest number in the county.
This year, four GSWs — medical shorthand for gunshot wounds — arrived on the first day of summer. One was a suicide and three were assaults. Three died and one would probably be discharged in a few days.
Now, on June 23, two more have come in, both teenagers, both assaults. They walked through the front door at 2:25 a.m., no EMTs, no police. Were you spending the night in the hospital, waiting for a shooting victim to come in? What was it like when one did come in? Relief? Fear?Barbara and I had spent three previous Saturdays at the hospital from 3 p.m. until 1 a.m., just waiting. We picked Saturdays, we picked the summer, we picked late nights because these are prime-time for shootings. On each occasion, nothing happened, and yes, we were surprised. It was our fourth night, around 2:15 a.m., and we were just about to call it quits – resigned to another night coming up with nothing – when these two boys walked into the emergency room. The chaos of their sudden arrival caught us off-guard, and suddenly we were off and running. With no time for reflection, for relief or fear, we were running with Dr. Putnam from the ER to the OR, changing into gowns, masks and boots and trying to stay out of the way.
The hospital staff calls it the homeboy ambulance service: patients brought in with injuries often from gang shootings.
Putnam can see that one of the boys will be OK. He has a clean wound through the shoulder.
The boy with the nickel-sized bullet hole is far worse, and they know nothing about him. No name, no age, no family. For now, they call him Zinc, one of the pseudonyms the hospital uses for its John Does.
Emergency departments in hospitals throughout America have physicians like Putnam, doctors who specialize in saving the lives of shooting victims.
Other traumas, like concussions and automobile accidents, can be subtle and require imaging to see what's hidden. Gun injuries don't hide their tracks, but they are just as much a mystery, a puzzle put together by the surgeon as seconds race by.
No matter the clarity of the injury, the damage can extend like concentric rings beyond the trajectory of the bullet. There is the blast effect, the sometimes fatal bruising that can occur to organs in the vicinity of a wound. There is the so-called triad of death, the interplay between body temperature, blood acidity and coagulation.
There is ancillary debris — shards of glass, pieces of clothing, even upholstery if the bullet has passed through furniture — and there are always infections from bacteria carried into the wound. Did your original drafts include more detail about this process? I’m sure books have been written about what bullets do to bodies, but you managed to tease out the essentials. How difficult was that?I wanted to keep it simple. I could have named the types of bacteria, even described various infections, but that would have cluttered, even interrupted the narrative. This boy was close to death, and I wanted to stay focused on this detail.
Putnam, 44, estimates that he has treated about 5,000 GSWs and consulted on nearly 2,000 more over the last 20 years, 10 of them at Harbor-UCLA. The victims he remembers the most are the children and women, the bystanders hit by stray fire, the wounded who spoke to him in the ER but died in the operating room.
Whenever he loses a patient, he hears his mother asking him what he could have done differently. And whenever he saves a life, he knows that success is often just a matter of luck.
Medicine and technology have come far in recent years in balancing the odds, but when it comes to gun violence, the numbers are overwhelming.
"Why guns?" Putnam asks. "Why so many guns? It once was fistfights. It once was stabbings. Now it's a whole new world out there, and with guns, it's just too much." In today’s world where guns and gun violence are such a serious and debated issue, this quote feels almost of a different, simpler time, before every news network had dissected congressional gun laws. Why did you include it?I was grateful that Dr. Putnam was as insightful as he was, and I liked this quote because it accomplished exactly what you describe. It reminds us of Dr. Putnam’s long experience with GSWs, and it takes us back to a more simple time, conveying in brief measure how quickly gun violence in America has grown out of hand.
The emergency room team washes the boy with an antiseptic. He has been intubated and anesthetized. Blood transfusions have begun.
"Sticky blues," Putnam calls out. No time to wait for the antiseptic to dry. Nurses drape blue cloths around the boy until he disappears, with only a torso remaining.
Putnam, dressed in surgical scrubs, gloves, cap and headlamp, makes the initial incision from sternum to pubic bone, bowing around the navel.
Chief resident Carrie Luu follows the scalpel with a "Bovie," a pen-shaped tool that cauterizes the open blood vessels with electrical current. Were these specifics of the operation confirmed after, or are you familiar with surgery and the tools needed?The surgery was chaotic, bloody and disorienting. In taking my notes, I tried to capture as best as I could what I was seeing. But there was a lot that I didn’t know: the materials, the procedures, the anatomy. I was lucky, however, to be standing beside an intern who answered my questions. When I got home later that morning, I typed my notes, capturing the fresh impressions as imprecise as they were. Then when I had a draft, I met with Dr. Putnam, and he and I talked through the particular moments of the surgery, filling in the details, capturing his impressions and fact-checking everything that I saw.
The air smells of singed flesh; tendrils of smoke rise into the lights. This is such a sickening and yet somehow beautiful combination of the senses. Can you talk about how you come up with such language?There is no forgetting the smell of singed flesh; it’s a memory that goes back to the first time we had a mishap with a burner on the stove or barbecue. But here it was at such an industrial scale, given the amount of cutting and cauterizing. And the lighting in the operating room was so cinematic, almost too bright, that the smoke was brilliantly illuminated as it moved and curled upward. As for “tendril,” it’s comes from – of all places – an art history class in college where the professor was describing cigarette posters from the Art Nouveau era. The artists loved to represent those languid strings of smoke, the tendrils, that patterned the air.
Putnam sets a clock running in his mind. Two hours is optimum. Three is the limit. Anything longer compounds the trauma with a phenomena known as physiologic exhaustion, when the body has worn itself out trying to compensate for the injury.
Putnam and Luu begin by separating the small intestine and colon from their ligaments. They notice a few holes in the bowel, but those repairs can come later.
Lifting the intestine out of the torso, they find a pool of blood the size of a football flooding the back of the abdomen. This explains why the entry wound was dry. The boy is losing more blood than they can give him. Putnam wonders again if they are too late. I feel now we are almost inside the mind of Putnam, with this level of detail and intimacy. Was he wondering this aloud? Did he tell you this after?Yes, this was the advantage of working with Dr. Putnam after the first draft was written. I was able to ask him about his feelings and thoughts during the surgery.
He orders more transfusions. A resident begins suctioning the abdomen.
"Minus 8," a nurse calls out. It's a measure of the blood's acidity, a reminder of the triad of death. A normal reading — zero — means blood clots can form naturally.
As patients lose blood, lactic acid accumulates in the cells, and the enzyme that helps coagulation doesn't function. The more acid, the more bleeding, and patients' temperatures drop until there's no stopping the loss.
Trauma teams try to interrupt this cycle. Transfusions and warming blankets help. The OR's thermostat is set as high as it will go: 85 degrees. The boy lies on a pad that's heated to 100 degrees, but still his temperature has fallen to 93.
Unable to see beyond the blood collecting in the abdomen, Putnam reaches in, and his fingers find the inferior vena cava — a vein nearly an inch in diameter — that channels blood from the lower half of the body back into the heart.
He pushes down on it, and the bleeding slows. When he eases up, he can hear a whoosh. The vena cava has been punctured.
Fired from a handgun, a .45-caliber bullet averages 900 feet per second, and unless it hits a bone, it usually follows a straight line.
This bullet's journey passed through the skin and the colon, the intestine and then the vena cava. It stopped just behind the pancreas, with its point boring nearly two inches into the spine at an angle, just missing the spinal cord.
Putnam probes the vertebra. He feels sharp fragments of bone and a hole in the L-3 vertebra no larger than his little finger. If the bullet posed a risk for pain or infection, he would remove it, but experience tells him it is safe to leave behind.
With the blood drained, he can see the damage to the vena cava: two holes in the vein, most of the tissue shredded. There will be no repairing it. Each end will have to be tied off permanently, and the other veins will have to adjust by carrying blood back to the heart.
But ligating the vena cava is tricky. Unlike arteries with their thick muscular walls, veins are as fragile as tissue paper.
Putnam puts a clamp with long pincers on the vein, which swells like a garden hose. In this graf and the one above, you’ve used everyday, relatable things to such great effect: tissue paper, a garden hose. Is that why you chose them, so people could really connect to what’s going on?That’s a nice observation, and yes, it’s true. When a story comes close to being technical (L-3 vertebra, vena cava, etc), I think it’s important for us to step away from the textbook and find an explanation, a picture, an analogy that renders the detail in the most ordinary terms possible. Not only does it make the reading experience effortless (critical for narratives, in my opinion), but it also represents my effort to help demystify the world, which – especially in the fields of science and medicine – has become so specialized as to be almost alienating. I think it’s incumbent on writers, narrative writers, to help break down those walls. Even in the best of circumstances, fewer than half of patients with similar injuries survive.
The boy jerks, a sudden reflex.
"Can you paralyze him so he'll stop bucking?" Putnam asks. This quote seems removed, almost inhumane. Do you think Putnam still sees all of the people he operates on as people?I believe that all surgeons understand that our bodies have minds of their own, and in this instance, like a broken machine, are subject to involuntary reflexes that can interfere with the business of living. In moments of such profound trauma, the body and soul become strangers to one another, which is natural and does not take away from our humanity.
More paralytics are added to the cocktail of intravenous drugs.
Putnam guides Luu, the chief resident, as she starts to tie off the vein. The stitch reverses direction with each pass and looks like the threads on a baseball.
"Minus 11," a nurse calls out. They have been working for almost 90 minutes.
"Come on," Putnam says, encouraging Luu. "This is where all these things really matter."
She is having trouble. Sideways torque in the needle tears out the suture. Luu is still learning — and Harbor-UCLA is a teaching hospital — but now Putnam has to take over.
"Big pledgets," he calls out, asking for the felt-like material, nearly an inch in diameter, that will act like gaskets to support each suture against the tissue. "Hurry, please."
His hands rise and fall quickly, deftly, with the grace of a pianist. His stitches, though, aren't perfect. He learned long ago that there was no call for elegance in surgeries like this. A perfect stitch could mean a dead patient.
With a little more than 12 passes, the lower portion of the vein is closed. They are almost two hours in. Putnam is sweating and splattered with blood. The room is stifling.
"Watch your eyes," Putnam announces as he removes the clamps and tests the sutures. Given the pressure in the vein, blood could spray across the room if the sutures don't hold. I love the commonsense yet ghoulish instructions. You convey information here in a simple yet dramatic way. How do you choose these moments?With every narrative, there is an inherent – and critical – tension between the action sequences (“Watch your eyes…”) and the exposition that explains why and helps orient the reader. I love playing with this rhythm, pushing the story ahead and then backing off, trying to gauge the reader’s capacity for each. Generally speaking, the stronger the action sequences, the easier it is to interrupt the flow with some explanation, which in my mind should always be – whenever possible – as brief as a haiku.
They hold.
"Still very oozy," he says. The body's normal coagulants haven't begun to stop the other sources of bleeding.
He and Luu staple the top portion of the vena cava and turn to the intestine. They draw the long, serpentine tube through their hands inch by inch, stapling and stitching any tear.
A cloth is tossed on the floor to mop the blood at Putnam's feet. By now, almost 80% of the boy's blood has been replaced.
Loosely positioning the intestine inside the abdomen, Putnam begins bandaging. He won't close the incision because he plans to open the boy again in two days to reassess the work and to see how the body is healing.
"OK, we're moving," the scrub tech announces as soon as Putnam steps back and begins to strip out of his surgical gown.
Putnam remembers all the bad news he's ever delivered. He won't have to remember this one. It strikes me that, for anybody other than a shooting-trauma surgeon, experiencing any part of this would be an unforgettable experience. What does it say about Putnam that he only remembers the ones that go wrong?It is common in emergency room setting that the doctors and nurses only remember the lives they were unable to save. These are the lives that are shrouded in the tears, in the wailing, the sudden outpouring of grief that comes when the family members learn the outcome in the waiting room. For Dr. Putnam, these memories are tied up with his own sorrow – and second-guessing – as he relives the surgeries that didn’t end favorably.
At 5:25 a.m., three hours after arrival, he pronounces the boy in critical condition, expected to live.
A little before 6 a.m., Putnam goes looking for the family. He still doesn't have any information about the boy.
Sleeping families fill the waiting rooms, and in the ER, Putnam speaks with the other victim, who says he doesn't know his friend's name.
Then a call comes in. A woman is asking if the hospital has seen a young man with the name Connie tattooed on the underside of his right arm.
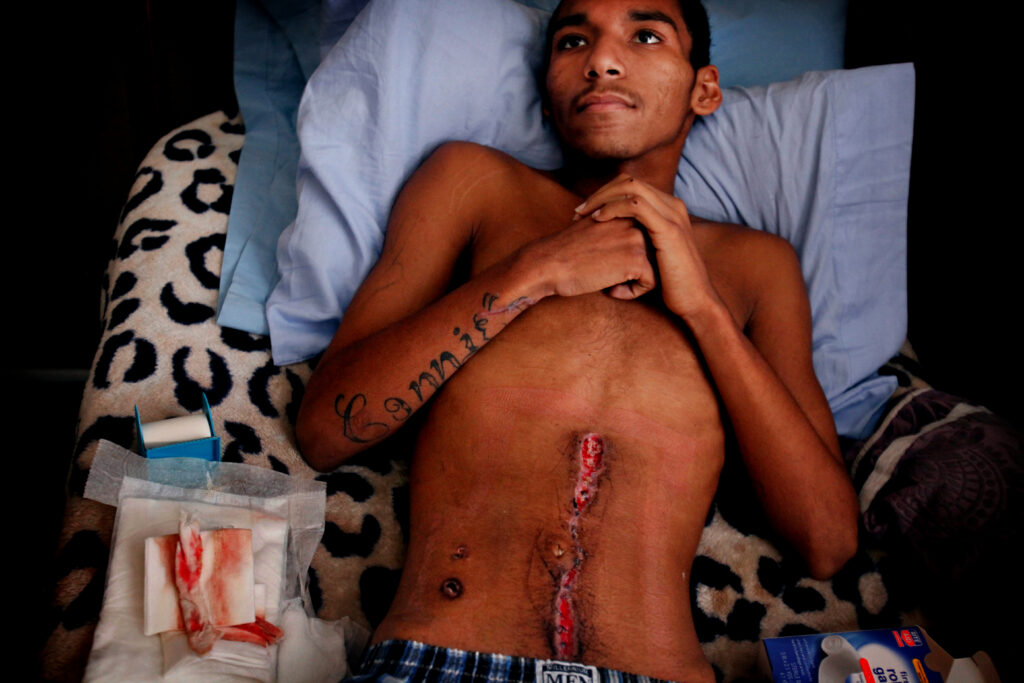
Within an hour, Connie Greene and her husband meet Putnam in the ICU. She is the boy's mother, and his name is Leandrus Benton. He is 16.
"He's OK," Putnam tells the parents. "He lost a lot of blood, and we almost lost him."
Connie starts to cry. In the last five years, two of her nephews have been killed in street shootings.
Leandrus — or Lee, as he's known to his family and friends — had been walking home from a party in Wilmington that night. As he would later explain, he and his friend thought it would be safer to take the alley than the street. Lee had heard the gun but didn't see the shooter. The bullet, he said, burned through his gut. Did you want to speak to Leandrus more, or his family? Or was the idea not to individualize the victim too much, since this is more a story about all shooting trauma victims and those who help them?That’s a good question, and you’re right. Of course I was tempted to tell more of Leandrus’ story, but when Barbara and I visited him at his home just a few days after he had been released from the hospital, he was weak and still in shock. And it didn’t feel right to do anything more than to introduce ourselves and explain what I wanted to do with this story. And, as I have noted, we have read about the gunshot victims before, and this is a story about Dr. Putnam, his skill, his training and his familiarity with the terrible things that guns can do. By association, I hope his story can help readers understand that gun violence isn’t just between the shooter and the shot, but that it touches dozens, if not hundreds, of other individuals who live in a world conscribed by reluctant politicians, the Second Amendment and the pain and suffering of neighborhoods where poverty and violence are so tragically interrelated.
Putnam walks the couple into the ICU, and as they wash their hands, he pulls out gowns, gloves and masks for them. He then takes them to Lee, waits a minute and draws the curtain around them so they can be alone with their son. The rhythm of the last words is lovely. I also like the image of the curtain, because the surgery was like theater, and the doctor is playing a role for a brief yet vital moment in the boy’s life, then steps away from it. Talk about choosing this ending.Writing is a collaborative art: Every writer needs an editor. I had two excellent editors on this piece, Drex Heikes, and Kari Howard, now editor of Storyboard, but both proposed a rewrite on my original. The first ending that I had written shifted the attention from the scene in the ICU to Putnam’s reflections on the night. I had wanted to use his words to channel my thoughts about the terrible relentlessness of these shootings. Clearly I was too close to the material. Drex and Kari felt that his quotes broke from the narrative and wanted me to try a subtler approach. So we decided instead to highlight this moment of tenderness and privacy, letting readers ask their own questions and walk away with their own sense of futility and perhaps sorrow.
Writer's note: Here is the original ending:
Within an hour, Connie Green and her husband meet Putnam in the ICU. The boy is 16 and his name is Leandrus Benton.
“He’s OK,” Putnam tells the parents. “He lost a lot of blood, and we almost lost him.”
Connie starts to cry. Two of her nephews had been killed in shootings in Long Beach.
Putnam walks the couple into the ICU and to their son’s bed. He draws a curtain around them.
They will learn later that Leandrus had been walking home from a party in Wilmington. He and his friend decided they would be safer to take the alley than the street. Leandrus heard a gun but didn’t see a shooter. A bullet suddenly burned like fire in his gut.
After being on duty nearly 24 hours, Putnam relaxes and reflects on the day.
“Traumas are random,” he says. “They leave you asking not just why did this happen, but – when things looked so bad – how did they turn around?
“It takes a lot of luck and the sense that someone is watching over us.”
Putnam is weary. “I just need to get through the shift,” he says.
But he knows that once he gets home, he will start wondering.
“Why guns? Why so many guns? Why do young people get status through guns? It once was fist fights. It once was stabbings. Now it’s a whole new world out there, and with guns, it’s just too much.”